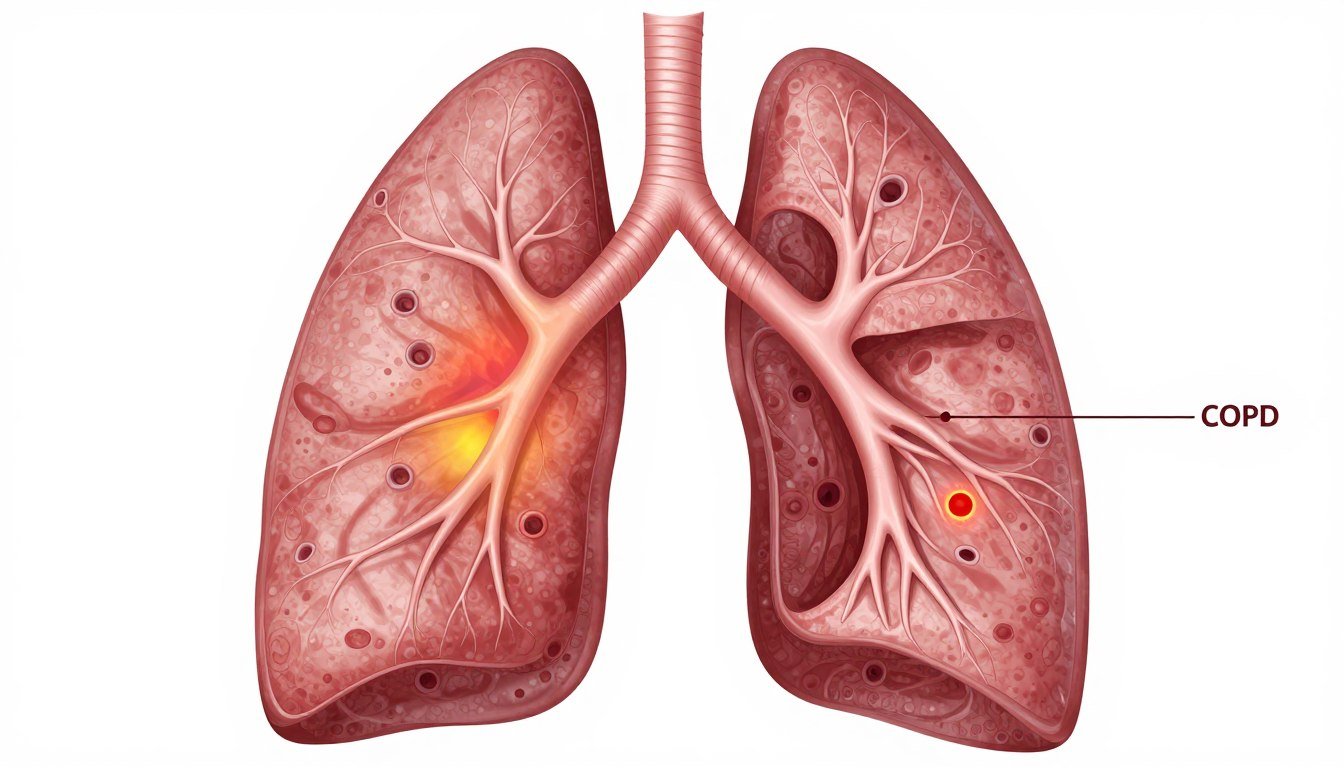
COPD (Chronic Obstructive Pulmonary Disease): Understanding America’s Silent Respiratory Crisis
Every breath you take is a gift. But for over 16 million Americans diagnosed with chronic obstructive pulmonary disease, breathing has become a daily struggle. COPD (Chronic Obstructive Pulmonary Disease) quietly affects millions more who remain undiagnosed.
This progressive lung disease doesn’t just impact breathing. It transforms lives, limits activities, and creates challenges for families across the United States.
Understanding COPD is the first step toward prevention, early detection, and effective management. This comprehensive guide explores everything you need to know about this serious respiratory condition.
Why Chronic Lung Disease Represents a Major Threat to US Health
Chronic obstructive pulmonary disease has emerged as one of America’s most pressing health challenges. The disease ranks as the fourth leading cause of death in the United States.
The economic burden is staggering. COPD costs the nation approximately $50 billion annually in direct healthcare expenses and lost productivity.
Beyond statistics, the human cost runs deeper. Millions of Americans experience reduced quality of life due to this chronic obstructive pulmonary condition.
Critical Fact: An estimated 12 million Americans have undiagnosed COPD, making early detection and screening essential for better health outcomes.
The disease burden continues growing. Several factors contribute to this alarming trend across the country.
Smoking remains the primary risk factor. However, occupational exposures and air pollution also play significant roles in disease development.
Healthcare systems face increasing pressure. Emergency department visits and hospitalizations for COPD complications strain medical resources nationwide.
Concerned About Your Lung Health?
Take our free COPD risk assessment and understand your respiratory health status. Early detection saves lives.
What is COPD (Chronic Obstructive Pulmonary Disease)?
COPD (Chronic Obstructive Pulmonary Disease) is a progressive lung disease that makes breathing increasingly difficult over time. The condition involves long-term obstruction of airflow in the lungs.
Two primary conditions fall under the COPD umbrella. These include emphysema chronic bronchitis, which often occur together in people with COPD.
Understanding the Two Main Types
Chronic bronchitis involves inflammation of the airways. The bronchial tubes become swollen and produce excess mucus that blocks air passages.
Emphysema affects the air sacs in the lungs. These tiny structures, called alveoli, become damaged and lose their elasticity over time.
Most people copd experience both conditions simultaneously. The combination creates the characteristic breathing difficulties associated with this obstructive pulmonary disease.
How COPD Affects Your Lungs
In healthy lungs, air flows freely through airways into air sacs. These delicate structures facilitate oxygen exchange with the bloodstream.
COPD damages this intricate system. Airways become inflamed and narrowed while air sacs lose their ability to expand and contract properly.
The result is trapped air in the lungs. This phenomenon makes it increasingly difficult to breathe out completely.
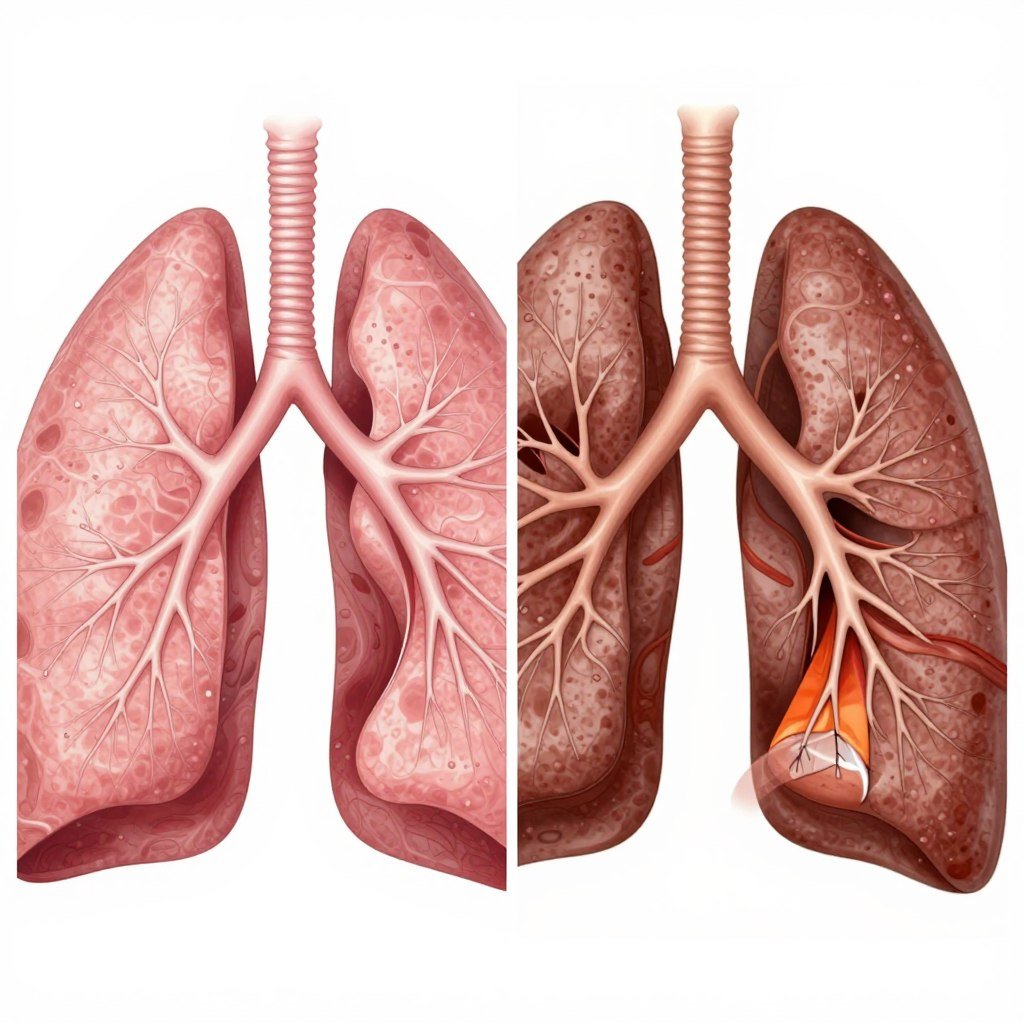
Medical Insight: Unlike asthma, COPD involves permanent lung damage. The condition is chronic and progressive, requiring long-term management strategies.
Age Groups Most Affected by COPD in the USA
Chronic obstructive pulmonary disease primarily affects middle-aged and older adults. The prevalence increases dramatically with age across American populations.
Primary Age Demographics
Adults aged 65 and older face the highest risk. Approximately 15% of Americans in this age group live with diagnosed COPD.
The 45-64 age bracket also shows significant prevalence. Early symptoms often emerge during these middle years as cumulative damage manifests.
Younger adults occasionally develop COPD. Early-onset cases often involve alpha-1 antitrypsin deficiency, a genetic condition affecting lung health.
Gender and Demographic Patterns
Women now represent the majority of people copd in America. This shift reflects changing smoking patterns over recent decades.
Rural populations face higher risk factors. Limited access to healthcare and higher smoking rates contribute to increased disease burden.
Socioeconomic factors play crucial roles. Lower-income communities experience disproportionate COPD rates due to environmental and occupational exposures.
| Age Group | Prevalence Rate | Primary Risk Factors | Diagnosis Rate |
| 18-44 years | 3.2% | Alpha-1 antitrypsin deficiency, early smoking | Low |
| 45-54 years | 6.8% | Cumulative smoking exposure, occupational hazards | Moderate |
| 55-64 years | 10.4% | Long-term smoking, environmental exposures | Moderate-High |
| 65+ years | 15.1% | Lifetime exposure accumulation, aging lungs | High |
Early detection remains challenging. Many younger adults attribute symptoms copd to aging or poor fitness rather than underlying lung disease.
How COPD Became Stressful and Out of Control in America
The chronic obstructive pulmonary disease crisis in America reflects decades of public health challenges. Multiple factors have converged to create this escalating situation.
The Smoking Legacy
Decades of tobacco use created a time bomb effect. Smoking remains the leading cause copd, responsible for 85-90% of all cases.
The peak smoking years of the 1950s through 1980s now manifest as current disease burden. Those who smoked heavily during these decades now face severe copd complications.
Despite declining smoking rates, the damage persists. Former smokers remain at higher risk for developing pulmonary disease years after quitting.
Environmental and Occupational Factors
Air quality concerns extend beyond smoking. Industrial pollution and environmental toxins contribute significantly to respiratory disease development.
Occupational exposures affect millions of workers. Construction, mining, and manufacturing jobs involve prolonged exposure to harmful dusts and chemicals.
Indoor air pollution poses hidden dangers. Biomass fuel burning and poor ventilation in homes increase risk factors for vulnerable populations.
Healthcare System Strain
Emergency departments see frequent COPD exacerbations. These acute episodes require immediate medical intervention and hospitalization.
Healthcare costs spiral upward. Each hospitalization for severe copd complications costs thousands of dollars in medical care.
The system struggles with preventive care. Focus remains on treating acute episodes rather than comprehensive disease management.
Diagnostic Challenges
Underdiagnosis remains a critical problem. Nearly half of all people copd remain unaware of their condition until advanced stages.
Symptoms are often dismissed initially. Patients and providers may attribute breathing difficulties to normal aging or deconditioning.
Delayed diagnosis worsens outcomes. Early intervention could slow disease progression and improve quality of life significantly.
Crisis Alert: COPD hospitalizations cost Medicare over $15 billion annually, with rates continuing to climb despite prevention efforts.
Comprehensive Prevention Strategies for COPD
Prevention remains the most effective approach to combating chronic obstructive pulmonary disease. Multiple strategies can significantly reduce your risk of developing this lung disease.
Smoking Cessation: The Primary Defense
Quitting smoking is the single most important step. This action dramatically reduces risk factors for developing obstructive pulmonary disease.
Even long-term smokers benefit from quitting. Lung function decline slows significantly within months of smoking cessation.
Support resources make quitting easier. Counseling, medications, and nicotine replacement therapies improve success rates substantially.
Immediate Benefits of Quitting
- Reduced airway inflammation within weeks
- Improved oxygen levels in bloodstream
- Decreased mucus production
- Lower risk of respiratory infections
- Slowed progression of existing lung damage
Long-term Protection
- Significantly reduced COPD development risk
- Better lung function preservation
- Improved overall health outcomes
- Extended life expectancy
- Enhanced quality of life
Environmental Protection Measures
Avoiding secondhand smoke exposure protects your airways. Even passive smoke exposure increases your risk of chronic obstructive pulmonary conditions.
Indoor air quality matters significantly. Use air purifiers and ensure proper ventilation in your living spaces.
Outdoor air pollution requires attention. Check air quality indexes and limit outdoor activities during high pollution days.
Occupational Safety Practices
Workplace exposure to dusts and chemicals demands protective measures. Proper respiratory equipment prevents harmful particle inhalation.
Follow safety protocols consistently. Regular equipment maintenance and proper usage protect your lungs during work hours.
Employer responsibilities include safe environments. Adequate ventilation systems and exposure monitoring protect worker respiratory health.
Vaccination and Infection Prevention
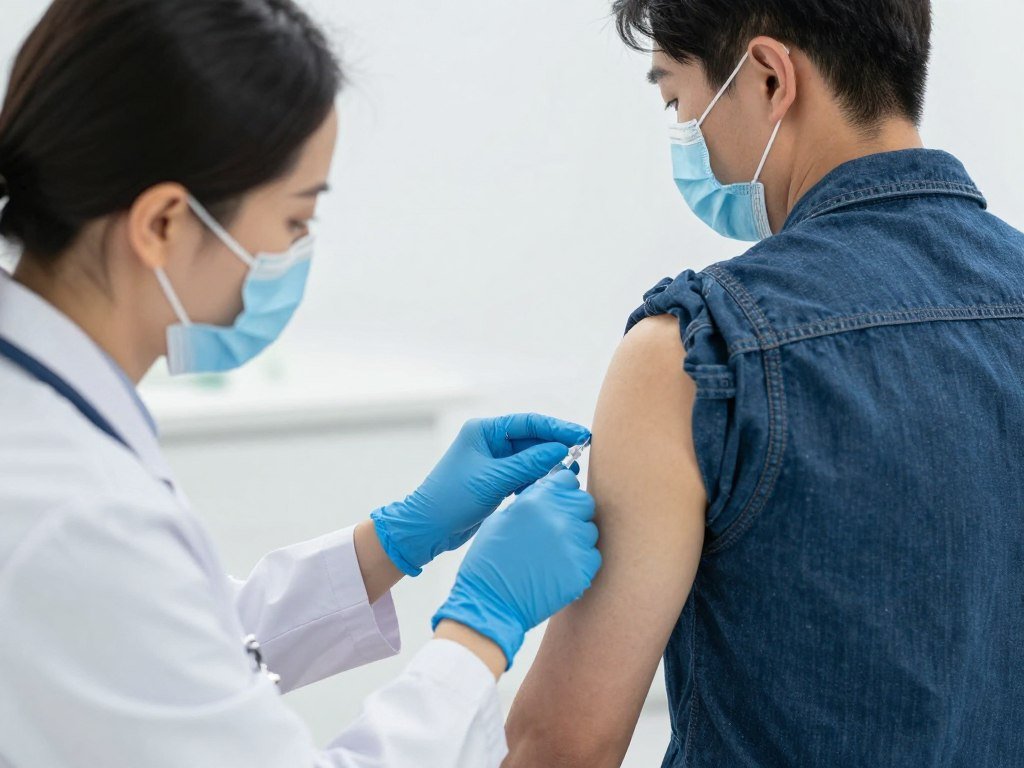
Annual flu vaccines reduce respiratory infections significantly. These preventive measures protect vulnerable airways from additional damage.
Pneumonia vaccination provides essential protection. This immunization prevents serious respiratory infections that could worsen lung function.
COVID-19 vaccination offers crucial defense. Respiratory infections pose serious risks for people with compromised lung health.
Early Detection Through Screening
Regular health checkups enable early identification. Spirometry testing measures lung function and detects early changes.
High-risk individuals need regular monitoring. Those with smoking history or occupational exposures should undergo periodic lung function assessments.
Symptom awareness prompts timely evaluation. Persistent cough, breathing difficulties, or excessive mucus production warrant medical attention.
Get Your Personalized Lung Health Action Plan
Download our comprehensive prevention guide with specific strategies tailored to your risk factors and lifestyle.
Is COPD Treatment Really Helpful? Medical Expert Insights
Treatment for chronic obstructive pulmonary disease has advanced significantly. Modern approaches can dramatically improve quality of life for people copd.
What Doctors Say About Treatment Outcomes
“While COPD cannot be cured, appropriate treatment significantly slows disease progression and improves patient outcomes. Early intervention combined with lifestyle modifications can add years of quality life.”
Medical professionals emphasize treatment effectiveness. Proper management reduces symptoms copd and prevents dangerous complications.
Pulmonary rehabilitation programs show remarkable results. These comprehensive programs combine exercise, education, and support for optimal outcomes.
Primary Treatment Approaches
Medication Therapy
Bronchodilators open airways and ease breathing difficulties. These medications reduce inflammation and help clear mucus from lungs.
Inhaled corticosteroids reduce inflammation in airways. Combined therapies work synergistically for better symptom control.
Oxygen Therapy
Supplemental oxygen improves blood oxygen levels. This treatment prevents complications from chronic low oxygen saturation.
Portable concentrators enable mobility. Modern technology allows oxygen therapy during daily activities and travel.
Pulmonary Rehabilitation
Structured exercise programs strengthen respiratory muscles. Breathing techniques improve oxygen efficiency during activities.
Education components empower patients. Knowledge about disease management leads to better adherence and outcomes.
Evidence-Based Treatment Benefits
Research demonstrates clear treatment advantages. Clinical studies show improved survival rates and reduced hospitalizations with proper care.
Advanced Treatment Options
Surgical interventions help select severe copd patients. Lung volume reduction surgery and transplantation offer options for advanced cases.
Bronchoscopic procedures provide less invasive alternatives. These techniques improve airflow without major surgery.
Emerging therapies show promise. Stem cell research and regenerative medicine may offer future treatment breakthroughs.
Doctor Perspectives on Treatment Timing
“The earlier we begin treatment, the better the outcomes. Patients who start therapy at mild or moderate stages experience significantly slower disease progression compared to those who delay treatment until severe symptoms develop.”
Medical consensus supports early intervention. Waiting until severe copd develops limits treatment effectiveness and recovery potential.

Pulmonary Rehabilitation Programs
Comprehensive programs combining exercise, education, and support for optimal COPD management and improved quality of life.

Oxygen Therapy Solutions
Advanced oxygen delivery systems that provide freedom and mobility while ensuring optimal oxygen levels for daily activities.
Medication Management
Personalized medication plans utilizing the latest bronchodilators and anti-inflammatory treatments for symptom control.
COPD Statistics Over 100 Years in America
Historical data reveals the evolution of chronic obstructive pulmonary disease in the United States. These statistics demonstrate changing patterns over the past century.
| Decade | Prevalence Rate | Annual Deaths | Major Contributing Factors | Healthcare Response |
| 1920s | 1.2% | ~15,000 | Industrial pollution, coal exposure | Limited awareness, minimal treatment |
| 1930s | 1.5% | ~22,000 | Increased smoking rates, workplace exposures | Basic oxygen therapy introduced |
| 1940s | 2.1% | ~35,000 | WWII industrial boom, smoking popularity | Recognition as distinct disease |
| 1950s | 3.4% | ~52,000 | Peak smoking era, air pollution | First bronchodilators developed |
| 1960s | 4.2% | ~68,000 | Continued high smoking rates | Pulmonary function testing standardized |
| 1970s | 4.8% | ~85,000 | Smoking consequences emerging | First surgeon general warnings |
| 1980s | 5.5% | ~96,000 | Aging smoker population | Improved inhaler technology |
| 1990s | 6.1% | ~112,000 | Legacy of smoking epidemic | Pulmonary rehabilitation programs expand |
| 2000s | 6.8% | ~124,000 | Continued smoking effects, aging population | Advanced combination therapies |
| 2010s | 6.4% | ~142,000 | Improved diagnosis, aging boomers | Personalized medicine approaches |
| 2020s | 6.0% | ~150,000 | COVID-19 complications, environmental factors | Telemedicine, targeted biologics |
The data reveals important trends. Prevalence peaked in the 2000s and has begun declining slightly due to reduced smoking rates.
However, absolute death numbers continue rising. The aging population means more people copd reach advanced disease stages.
Modern diagnosis improvements explain some changes. Better detection methods identify more cases earlier in disease progression.
Is COPD Reversible or Chronic? Understanding the Disease Nature
One of the most common questions patients ask concerns COPD reversibility. Understanding the chronic nature of this obstructive pulmonary disease is essential for realistic expectations.
The Chronic Reality
COPD is a chronic, progressive condition. The lung damage characteristic of emphysema chronic bronchitis cannot be completely reversed.
Permanent structural changes occur in airways and air sacs. Once these delicate structures are damaged, they cannot regenerate to normal function.
This differs fundamentally from reversible conditions like asthma. While asthma involves temporary airway narrowing, COPD causes permanent tissue damage.
What Can Improve
- Symptom severity and frequency
- Breathing capacity and ease
- Exercise tolerance and stamina
- Quality of daily life
- Progression rate can slow dramatically
- Exacerbation frequency reduces
- Oxygen levels can stabilize
What Cannot Reverse
- Destroyed air sacs in emphysema
- Permanent airway scarring
- Loss of lung elasticity
- Structural airway changes
- Thickened airway walls
- Damaged cilia function
Hope Through Management
While not reversible, COPD is highly manageable. Proper treatment dramatically improves symptoms and slows progression.
Early intervention makes the biggest difference. Starting treatment before severe copd develops preserves more lung function.
Smoking cessation remains paramount. Quitting smoking at any disease stage slows further damage and improves outcomes.
The Progressive Nature
Without treatment, chronic obstructive pulmonary disease worsens over time. Lung function gradually declines as damage accumulates.
Treatment changes this trajectory. Appropriate care can slow progression to nearly normal aging rates in some patients.
Individual responses vary considerably. Genetics, adherence to treatment, and overall health affect disease progression rates.
Important Understanding: While COPD cannot be cured or reversed, many patients live active, fulfilling lives with proper management. The key is early diagnosis and consistent treatment adherence.
Lifestyle Habits That Lead to COPD Development
Certain lifestyle choices significantly increase your risk of developing chronic obstructive pulmonary disease. Understanding these risk factors helps guide prevention strategies.
Smoking: The Primary Culprit
Cigarette smoking causes 85-90% of all COPD cases. This single risk factor dominates all others in disease development.
Tobacco smoke damages airways directly. The thousands of chemicals in smoke destroy air sacs and cause chronic inflammation.
Duration and intensity both matter. Pack-years (packs per day multiplied by years smoking) directly correlate with disease risk.
Smoking Impact Levels
- Light Smokers (under 10 pack-years): 2-3 times higher risk than non-smokers
- Moderate Smokers (10-20 pack-years): 5-7 times higher risk of COPD development
- Heavy Smokers (over 20 pack-years): 10-15 times higher risk, often developing severe copd
- Very Heavy Smokers (over 40 pack-years): Nearly certain to develop some degree of obstructive pulmonary disease
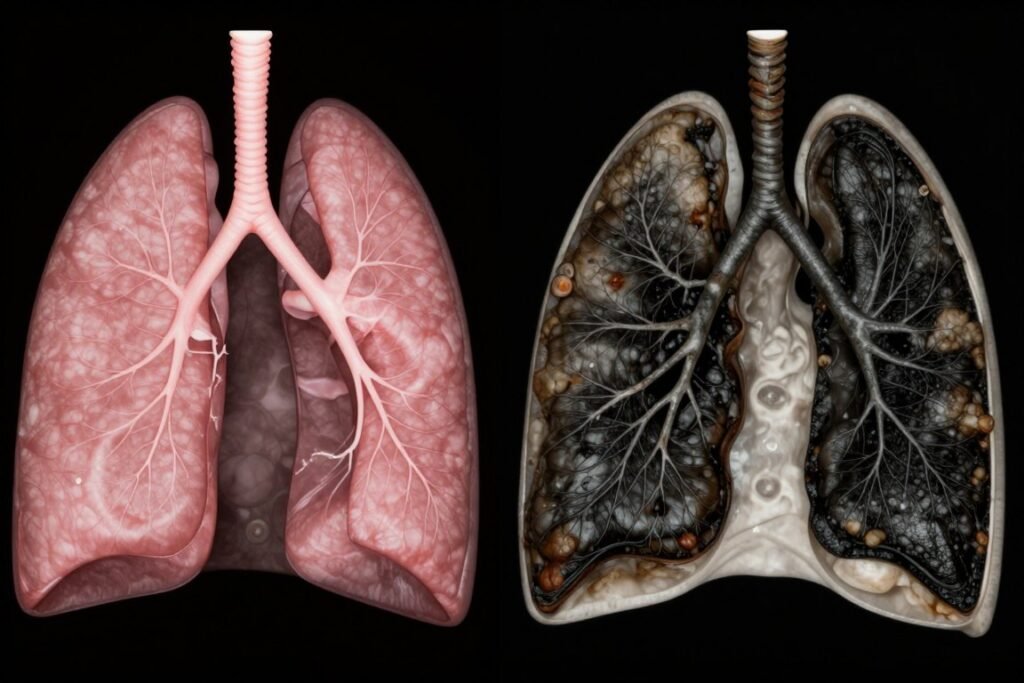
Secondhand Smoke Exposure
Passive smoke exposure carries significant risks. Living with smokers or working in smoking environments damages lungs progressively.
Children exposed to secondhand smoke face higher risk. Early childhood exposure affects lung development and increases adult COPD susceptibility.
No safe level of secondhand smoke exists. Even occasional exposure contributes to cumulative lung damage over time.
Occupational Exposures
Workplace hazards contribute to 15-20% of COPD cases. Certain professions carry substantially higher risk for developing pulmonary disease.
- Coal mining and mineral extraction
- Construction and demolition work
- Manufacturing with chemical exposure
- Agricultural work with organic dusts
- Textile industry workers
- Welding and metalworking
High-Risk Occupations
- Silica dust from stone cutting
- Asbestos fibers in older buildings
- Chemical fumes and vapors
- Grain and cotton dust
- Coal dust and diesel exhaust
- Cadmium and welding fumes
Dangerous Exposures
Environmental Air Pollution
Long-term exposure to outdoor air pollution increases COPD risk. Vehicle emissions, industrial pollution, and particulate matter damage airways gradually.
Indoor air quality affects health significantly. Biomass fuel burning for cooking and heating in poorly ventilated spaces causes substantial harm.
Urban living presents challenges. Higher pollution levels in cities correlate with increased respiratory disease prevalence.
Genetic Predisposition
Alpha-1 antitrypsin deficiency represents the primary genetic risk factor. This genetic condition affects protein production that protects lungs.
Approximately 1-3% of COPD cases involve this genetic condition. Affected individuals develop disease earlier and more severely than others.
Family history matters even without identified genetic mutations. Having relatives with COPD increases your personal risk substantially.
Additional Contributing Factors
Childhood respiratory infections impact adult lung health. Severe infections during development may increase later COPD susceptibility.
Socioeconomic factors influence disease risk. Limited healthcare access, poor nutrition, and substandard housing conditions contribute to higher rates.
Poor overall health habits compound risks. Inadequate nutrition, sedentary lifestyle, and untreated health conditions worsen outcomes.
Habits That Can Improve Lung Health and Function
Positive lifestyle changes can significantly improve respiratory health. These habits benefit everyone, especially those at higher risk for chronic obstructive pulmonary disease.

Regular Physical Exercise
Aerobic exercise strengthens respiratory muscles. Regular activity improves oxygen efficiency and overall breathing capacity.
Start gradually and build endurance. Even modest exercise provides benefits for people copd and those at risk.
Pulmonary rehabilitation programs offer structured approaches. These supervised programs combine exercise with education for optimal results.
Cardiovascular Exercise
- Walking 30 minutes daily
- Swimming for low-impact conditioning
- Cycling to build stamina
- Dancing for enjoyable activity
Breathing Exercises
- Pursed-lip breathing technique
- Diaphragmatic breathing practice
- Deep breathing exercises
- Coordinated breathing patterns
Strength Training
- Upper body exercises
- Core strengthening routines
- Resistance band workouts
- Light weight training
Proper Nutrition for Lung Health
Balanced nutrition supports respiratory function. Specific nutrients help reduce inflammation and support immune health.
Antioxidant-rich foods protect airways. Fruits and vegetables provide vitamins that combat oxidative stress in lungs.
Adequate protein intake maintains muscle strength. Respiratory muscles need proper nutrition for optimal function.

Lung-Healthy Foods
- Leafy green vegetables rich in antioxidants
- Fatty fish containing omega-3 fatty acids
- Berries packed with protective compounds
- Nuts and seeds for vitamin E
- Citrus fruits for vitamin C
- Tomatoes containing lycopene
- Green tea with anti-inflammatory properties
Breathing Technique Practices
Pursed-lip breathing slows respiration rate. This technique keeps airways open longer and improves gas exchange.
Diaphragmatic breathing strengthens the primary respiratory muscle. Regular practice improves breathing efficiency significantly.
Controlled breathing during activities conserves energy. Learning to coordinate breathing with movement reduces breathlessness.
Environmental Optimization
Clean indoor air quality protects airways. Use air purifiers and maintain proper ventilation in living spaces.
Avoid respiratory irritants consistently. Chemical fumes, strong perfumes, and cleaning products can trigger symptoms.
Humidity levels matter for comfort. Maintaining 30-50% relative humidity prevents airway drying and mucus problems.
Infection Prevention Strategies
Hand washing prevents respiratory infections. Regular hygiene reduces exposure to viruses and bacteria.
Stay current with vaccinations. Flu, pneumonia, and COVID-19 vaccines protect vulnerable airways from infections.
Avoid crowded spaces during illness seasons. Limiting exposure to respiratory infections protects lung health.
Stress Management and Sleep
Chronic stress affects breathing patterns. Relaxation techniques like meditation improve respiratory control.
Quality sleep supports immune function. Adequate rest helps the body repair and maintain healthy tissues.
Proper sleeping positions aid breathing. Elevating the head reduces nighttime breathing difficulties.
Hydration for Respiratory Health
Adequate water intake thins mucus. Proper hydration makes clearing airways easier and more effective.
Aim for 8-10 glasses daily. Individual needs vary based on activity level and climate.
Avoid excessive caffeine and alcohol. These substances can cause dehydration and worsen breathing issues.
Frequently Asked Questions About COPD
What are the earliest warning signs of COPD?
Early symptoms copd include persistent cough lasting more than three weeks, increased mucus production, shortness of breath during routine activities, and frequent respiratory infections. Many people dismiss these signs as normal aging or being “out of shape.”
Wheezing, chest tightness, and fatigue also indicate potential problems. If you experience these symptoms, especially with smoking history, consult a healthcare provider for lung function testing.
Can you live a normal life with COPD?
Yes, many people copd live active, fulfilling lives with proper management. Treatment advances allow patients to control symptoms effectively and maintain good quality of life.
Success depends on early diagnosis, medication adherence, pulmonary rehabilitation participation, and lifestyle modifications. While COPD is chronic, it doesn’t have to severely limit your activities with appropriate care.
How quickly does COPD progress?
Progression rates vary significantly among individuals. Without treatment, lung function typically declines faster than normal aging. However, proper management can slow progression dramatically.
Smoking cessation is crucial – it slows decline to near-normal rates in many patients. Regular monitoring, medication compliance, and lifestyle changes all influence how quickly chronic obstructive pulmonary disease advances.
Is COPD hereditary?
While most COPD results from environmental exposures, genetic factors play a role. Alpha-1 antitrypsin deficiency is the primary genetic condition causing COPD, affecting 1-3% of patients.
Family history increases risk even without identified genetic mutations. If relatives have COPD, you face higher risk and should avoid smoking and occupational exposures more carefully.
What’s the difference between COPD and emphysema?
COPD is an umbrella term covering several conditions, while emphysema is one specific type. Emphysema involves destruction of air sacs in the lungs, causing permanent damage.
Most patients have both emphysema chronic bronchitis simultaneously. Chronic bronchitis involves airway inflammation and mucus production. Together, these conditions create the breathing difficulties characteristic of chronic obstructive pulmonary disease.
Should I use supplemental oxygen?
Oxygen therapy benefits patients with chronically low blood oxygen levels. Your doctor determines need through pulse oximetry and arterial blood gas testing.
If prescribed, oxygen therapy improves survival and quality of life. Modern portable concentrators allow mobility and normal activities. Never adjust oxygen flow rates without medical guidance.
Taking Action Against COPD
Chronic obstructive pulmonary disease represents a significant health challenge. However, understanding this condition empowers you to take protective action.

Prevention remains the most effective strategy. Avoiding smoking, protecting yourself from occupational hazards, and maintaining overall health reduce your risk dramatically.
For those already diagnosed, hope exists through treatment. Modern therapies slow progression and improve symptoms significantly when started early.
The key to success lies in proactive health management. Regular checkups, symptom awareness, and prompt medical attention enable early intervention.
Don’t wait until breathing becomes severely compromised. Taking action today protects your respiratory health for years to come.
Your lungs deserve the same attention you give your heart. Prioritize respiratory health through informed choices and professional guidance.