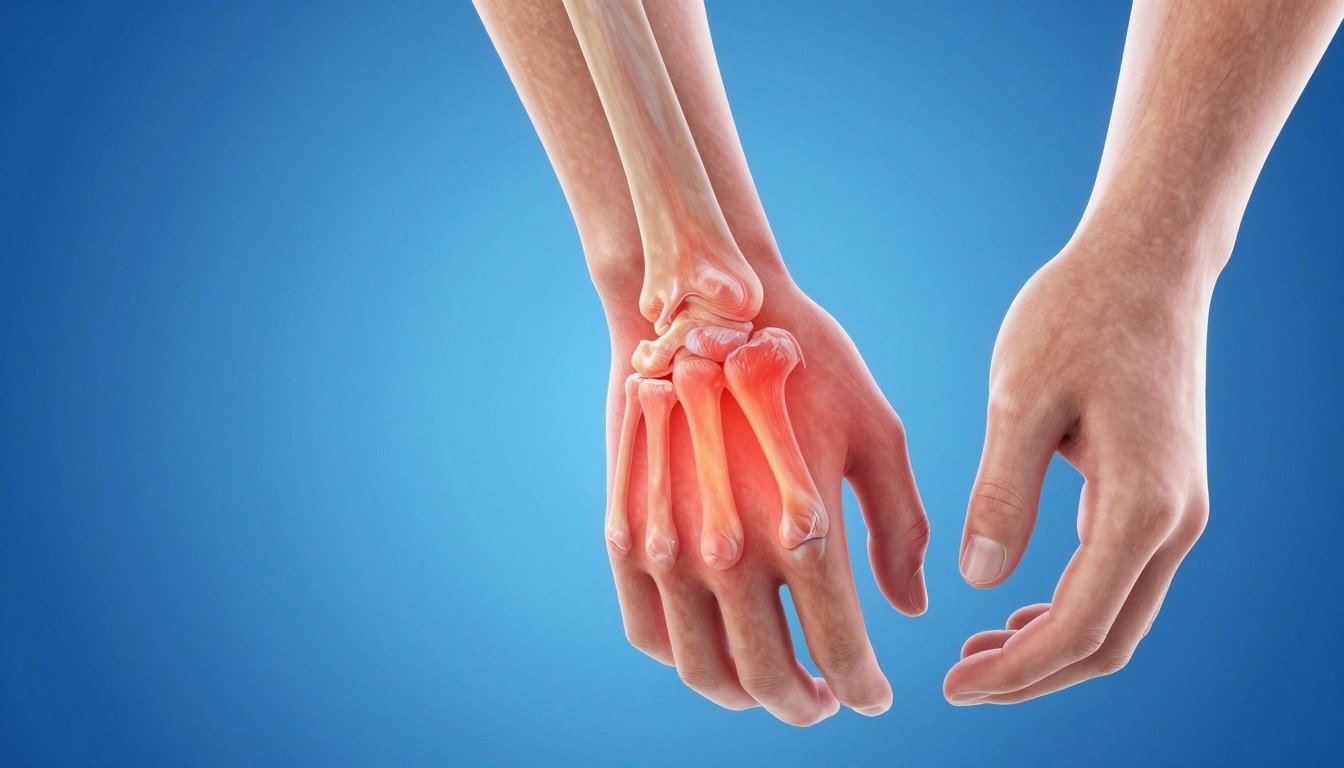
Understanding Arthritis: America’s Silent Epidemic Affecting Millions
Every day, millions of Americans wake up with joint pain that affects their ability to work, play with their children, or simply walk without discomfort. Arthritis has become one of the most significant health challenges facing the United States. This condition silently impacts the lives of more than 58 million adults across the country.
The burden extends far beyond physical pain. Arthritis represents a major economic and social crisis that demands our immediate attention. Understanding this disease is the first step toward protecting your joints and maintaining your quality of life for years to come.
What Is Arthritis? Defining This Complex Joint Condition
Arthritis is not a single disease but rather an umbrella term describing over 100 different conditions that cause inflammation and damage to joints throughout the body. The word arthritis literally means “joint inflammation.” This inflammation leads to pain, stiffness, swelling, and decreased range of motion in affected areas.
The Most Common Forms of Arthritis
While there are many types of arthritis, several forms affect the largest number of people in the United States. Each type has unique characteristics and causes different levels of joint damage over time.
Osteoarthritis
Osteoarthritis represents the most common type arthritis affecting over 32 million Americans. This form occurs when the protective cartilage cushioning the ends of bones gradually wears away over time. The bones begin rubbing together, causing pain and stiffness.
- Most frequently affects knees, hips, hands, and spine
- Develops slowly over many years
- Often related to aging and joint overuse
- Can result from previous joint injuries
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease where the immune system mistakenly attacks healthy joint tissue. This type arthritis causes inflammation that can damage joints and organs throughout the body. About 1.5 million Americans live with this condition.
- Affects joints on both sides of the body symmetrically
- Can develop at any age, even in children
- Causes systemic inflammation beyond joints
- Requires ongoing medical management
Other Significant Types Arthritis
Beyond the two most common forms, several other types arthritis significantly impact American health. Psoriatic arthritis affects people with the skin condition psoriasis, causing joint inflammation along with skin symptoms. This condition affects approximately 30% of people who have psoriasis.
Ankylosing spondylitis primarily targets the spine, causing inflammation where tendons and ligaments attach to bones. Over time, this can lead to fusion of the vertebrae. Gout represents another painful form where uric acid crystals accumulate in joints, most commonly affecting the big toe.
Juvenile idiopathic arthritis describes various forms of arthritis that develop in children under age 16. This condition can affect growth and development, making early diagnosis and treatment especially important for young patients.
Why Arthritis Is a Major Threat to US Health and Economy
The scale of the arthritis crisis in America cannot be overstated. This disease affects more people than diabetes and heart disease combined. Current data shows that one in four adults in the United States lives with doctor-diagnosed arthritis. The numbers continue climbing each year.
The Growing Burden on American Health
Arthritis stands as the leading cause of disability in the United States. The condition limits daily activities for more than 24 million Americans. These people struggle with basic tasks like climbing stairs, walking short distances, or even getting dressed without assistance.
The pain and stiffness associated with arthritis forces many people to reduce their physical activity. This inactivity creates a dangerous cycle. Less movement leads to weaker muscles, reduced flexibility, and increased joint damage. The resulting physical decline accelerates other health problems including obesity, heart disease, and diabetes.
Critical Fact: Arthritis causes more than 1 million hospitalizations and 45 million outpatient visits annually. The healthcare system struggles to manage this overwhelming demand while millions suffer from inadequate access to specialized care.
Economic Impact: The Hidden Cost Crisis
The financial burden of arthritis extends far beyond medical bills. Total costs associated with arthritis and related conditions exceed $300 billion annually in the United States. This figure includes both direct medical expenses and lost wages from missed work.
People with arthritis face higher healthcare costs throughout their lives. They require more frequent doctor visits, prescription medications, physical therapy sessions, and sometimes surgical interventions. Many also need assistive devices like braces, canes, or mobility scooters.
Lost productivity represents another massive economic drain. Workers with arthritis miss more days of work than those without the condition. Many are forced to reduce their working hours or leave the workforce entirely due to physical limitations. This affects not only individual families but also employers and the broader economy.
Workplace Impact: Arthritis results in approximately 172 million lost workdays each year. Employers face increased costs from reduced productivity, disability claims, and the need to accommodate workers with physical limitations.

Contrary to popular belief, arthritis does not only affect elderly people. While the risk certainly increases with age, this disease impacts Americans across all age groups. Understanding which populations face the highest risk helps target prevention efforts more effectively.
Adults Ages 65 and Older: The Highest Risk Group
More than half of all Americans age 65 and older have been diagnosed with some form of arthritis. This represents approximately 32 million people in this age bracket alone. The prevalence of osteoarthritis increases dramatically after age 50 as cumulative joint wear becomes more apparent.
Older adults face unique challenges managing arthritis symptoms. Many have multiple chronic conditions that complicate treatment. The pain and stiffness often lead to reduced mobility, increasing their risk of falls, fractures, and loss of independence.
Middle-Aged Adults: The Overlooked Population
Adults between ages 45 and 64 represent a substantial portion of arthritis cases. Approximately 31% of people in this age group live with the condition. This is the prime working age, making the economic and productivity impacts especially significant.
Many middle-aged adults dismiss early arthritis symptoms as normal aging or temporary injuries. This delay in seeking treatment allows joint damage to progress unnecessarily. Early intervention during this stage could prevent more serious complications later in life.
Young Adults and Children: An Emerging Concern
Arthritis also affects younger populations more frequently than most people realize. About 7.1% of adults ages 18 to 44 have been diagnosed with arthritis. Young people with inflammatory types arthritis like rheumatoid arthritis or psoriatic arthritis face decades of disease management ahead.
Juvenile idiopathic arthritis affects approximately 300,000 children in the United States. These young patients must navigate school, sports, and social activities while managing chronic pain and medical treatments. The psychological impact can be substantial during these formative years.
Risk Factors by Age Group
Different age groups face distinct risk factors that contribute to arthritis development:
- Younger adults: Sports injuries, autoimmune conditions, genetic factors
- Middle-aged adults: Obesity, occupational stress on joints, previous injuries
- Older adults: Cumulative joint wear, reduced cartilage regeneration, bone changes
- All ages: Family history, inflammatory conditions, joint abnormalities
How Arthritis Becomes Overwhelming and Out of Control in America
The journey from initial diagnosis to feeling overwhelmed by arthritis happens gradually for most people. The chronic nature of this disease creates ongoing stress that affects every aspect of life. Understanding how arthritis spirals out of control helps identify intervention points.

The Physical Decline Cycle
Arthritis creates a vicious cycle that accelerates physical decline. Joint pain makes movement uncomfortable, so people naturally reduce their activity levels. This decreased movement weakens the muscles supporting affected joints. Weaker muscles provide less joint stability, leading to more pain and further damage.
The inflammation associated with many forms of arthritis also causes systemic effects throughout the body. Chronic inflammation contributes to cardiovascular disease, depression, and other health conditions. These additional problems compound the difficulties of managing arthritis effectively.
Psychological and Emotional Burden
Living with chronic pain takes a severe emotional toll. People with arthritis report higher rates of depression and anxiety compared to the general population. The constant discomfort disrupts sleep, affecting mood and mental clarity during waking hours.
Many individuals experience grief over lost abilities. Activities they once enjoyed become difficult or impossible. Social isolation increases as people withdraw from activities that cause pain or embarrassment about physical limitations.
Mental Health Alert: Studies show that adults with arthritis are twice as likely to experience serious psychological distress compared to those without the condition. This mental health component requires attention alongside physical symptoms for comprehensive care.
Healthcare System Challenges
Many Americans struggle to access appropriate arthritis care. There is a shortage of rheumatologists and orthopedic specialists in many regions, especially rural areas. Wait times for appointments can stretch for months, during which joint damage progresses.
The complexity of arthritis treatment also contributes to poor outcomes. Managing the condition often requires coordination between multiple healthcare providers. Communication gaps between doctors can lead to conflicting advice or medication interactions.
High costs create additional barriers. Even with insurance, copays for specialist visits, medications, and treatments add up quickly. Some people ration medications or skip recommended therapies due to financial constraints, allowing their condition to worsen unnecessarily.
Social and Financial Stress Factors
Work limitations create financial stress for many arthritis patients. Those who continue working often struggle to maintain performance while managing symptoms. Workplace accommodations may be inadequate or unavailable, forcing difficult decisions about career continuation.
Family relationships also suffer under the strain of chronic illness. Partners may need to take on caregiving responsibilities. Parents with arthritis worry about their ability to care for children. The role changes create tension and guilt within households.
Effective Prevention: Can We Stop Arthritis Before It Starts?

While some risk factors for arthritis cannot be changed, many aspects of the disease can be prevented or delayed through proactive measures. Prevention strategies work best when implemented early, before significant joint damage occurs.
Weight Management: The Single Most Important Factor
Maintaining a healthy body weight represents the most effective modifiable factor for preventing osteoarthritis, especially in weight-bearing joints like knees and hips. Each pound of excess body weight puts approximately four pounds of extra pressure on knee joints during walking.
Studies show that losing just 10 to 12 pounds can reduce arthritis pain by 50% in people who are overweight. Weight loss also decreases inflammation throughout the body, which helps protect against inflammatory types arthritis as well.
Regular Physical Activity and Exercise
Exercise strengthens the muscles supporting joints, improving stability and reducing stress on cartilage. Regular movement also maintains flexibility and range of motion. Contrary to old beliefs, appropriate exercise does not wear out joints but actually protects them.
The best exercises for joint health include low-impact activities that minimize stress while maximizing movement. Swimming, water aerobics, cycling, and walking provide excellent cardiovascular benefits without excessive joint strain. Strength training builds muscle mass that cushions and supports joints.
Recommended Activities
- Swimming and water exercises
- Walking on level surfaces
- Stationary cycling
- Tai chi and yoga
- Light resistance training
- Stretching and flexibility work
Activities to Approach Carefully
- Running on hard surfaces
- High-impact aerobics
- Contact sports
- Activities with jumping
- Heavy weightlifting
- Repetitive high-stress movements
Joint Protection and Injury Prevention
Previous joint injuries significantly increase arthritis risk later in life. Protecting joints from trauma helps prevent post-traumatic arthritis. This includes using proper techniques during sports and physical activities, wearing appropriate protective equipment, and addressing injuries promptly.
Occupational factors also play a role. Jobs requiring repetitive motions or heavy lifting stress joints over time. Using proper body mechanics, taking regular breaks, and employing assistive devices can reduce cumulative damage to joints throughout a working career.
Nutrition and Anti-Inflammatory Diet
Certain dietary patterns may help reduce inflammation and protect joint health. An anti-inflammatory diet emphasizes fruits, vegetables, whole grains, fatty fish, and healthy fats while limiting processed foods, red meat, and added sugars.
Specific nutrients show particular promise for joint health. Omega-3 fatty acids found in fish oil have anti-inflammatory properties. Vitamin D supports bone health and immune system function. Antioxidants in colorful fruits and vegetables combat oxidative stress that damages cells.
Early Detection and Intervention
Catching arthritis in its earliest stages allows for interventions that can slow or even halt progression. People with family history of arthritis or other risk factors should monitor for early warning signs including persistent joint pain, morning stiffness lasting more than 30 minutes, or swelling that does not resolve quickly.
Seeking medical evaluation at the first signs of symptoms enables earlier treatment initiation. Many disease-modifying treatments work best when started before extensive joint damage has occurred.
Is Arthritis Treatment Really Helpful? What Results Can You Expect?
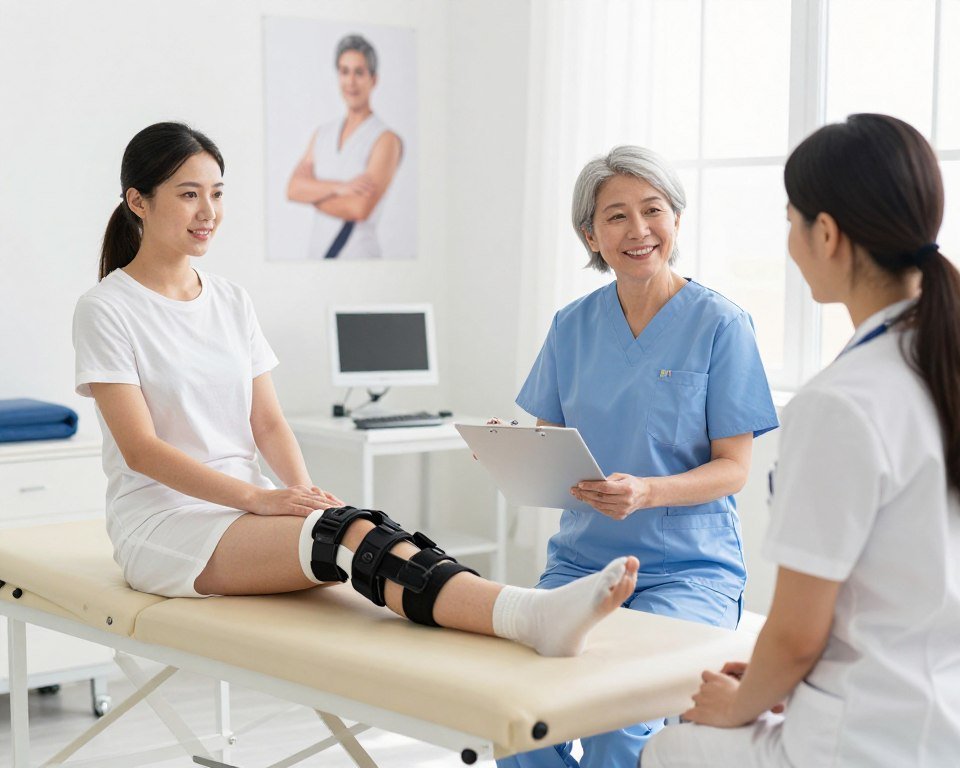
The effectiveness of arthritis treatment has improved dramatically over recent decades. Modern treatments cannot cure most forms of arthritis, but they can significantly reduce symptoms, slow disease progression, and help people maintain active lifestyles far longer than was possible in the past.
Treatment Effectiveness Depends on Type and Timing
Treatment success varies considerably based on the type arthritis and how early intervention begins. Inflammatory types arthritis like rheumatoid arthritis respond particularly well to modern disease-modifying medications when treatment starts early. These drugs can prevent joint damage and maintain function for many years.
Osteoarthritis treatment focuses more on symptom management and slowing progression since cartilage does not regenerate once lost. However, comprehensive treatment programs combining multiple approaches produce meaningful improvements in pain and function for most people.
Medication Options and Their Results
Various medications address different aspects of arthritis. Over-the-counter pain relievers help manage mild to moderate symptoms. Prescription medications offer stronger options for those with more severe pain or inflammation.
Disease-modifying antirheumatic drugs (DMARDs) have revolutionized treatment for rheumatoid arthritis and other inflammatory conditions. These medications target the immune system to reduce inflammation and prevent joint damage. Most patients experience significant improvement within three to six months of starting treatment.
Biologic medications represent the newest class of arthritis drugs. These treatments target specific immune system proteins involved in inflammation. Biologics often help people who have not responded adequately to other treatments. Blood tests help doctors monitor response and adjust medications as needed.
Physical Therapy and Rehabilitation
Physical therapy plays a crucial role in arthritis management. Trained therapists teach exercises that strengthen muscles around affected joints, improve flexibility, and increase range of motion. Many patients report reduced pain and improved function after completing physical therapy programs.
Occupational therapy helps people adapt daily activities to reduce joint stress. Therapists recommend assistive devices and teach joint protection techniques. These practical strategies allow people to maintain independence while minimizing pain and preventing further damage.
Surgical Interventions
Surgery becomes necessary when conservative treatments no longer provide adequate relief. Joint replacement surgery has become increasingly successful, with most patients experiencing dramatic pain reduction and functional improvement. Hip and knee replacements represent some of the most successful surgical procedures in modern medicine.
Less invasive surgical options may help in earlier disease stages. Arthroscopy allows surgeons to remove damaged tissue, repair tears, or smooth rough cartilage. These procedures often provide relief and may delay the need for more extensive surgery later.
Integrative and Complementary Approaches
Many people find additional relief through complementary treatments used alongside conventional medical care. Acupuncture, massage therapy, and mindfulness meditation show benefits in clinical studies. These approaches work best as part of a comprehensive treatment plan rather than as standalone therapies.
Dietary supplements receive significant attention for arthritis, though scientific evidence varies. Glucosamine and chondroitin show modest benefits for some people with osteoarthritis. Turmeric and ginger possess anti-inflammatory properties that may reduce symptoms when used consistently over time.
What Doctors Say About Arthritis Management and Outlook

Medical experts emphasize that arthritis management requires a comprehensive, individualized approach. No single treatment works for everyone. The most successful outcomes occur when patients and healthcare providers work together to develop personalized care plans.
Expert Consensus on Treatment Approaches
Leading rheumatologists stress the importance of early aggressive treatment for inflammatory arthritis conditions. The medical community has shifted toward a “treat-to-target” strategy, where doctors adjust medications to achieve specific goals like minimal disease activity. This approach prevents joint damage more effectively than older treatment philosophies.
For osteoarthritis, doctors recommend starting with conservative measures before progressing to more aggressive interventions. The American College of Rheumatology guidelines emphasize exercise, weight management, and physical therapy as first-line treatments. Medications and surgery come into play when these approaches provide insufficient relief.
The Importance of Patient Engagement
Healthcare providers consistently note that patient engagement dramatically affects outcomes. People who actively participate in their care, follow treatment recommendations, and communicate openly with their medical team achieve better results than passive patients.
Doctors emphasize that arthritis management extends far beyond the clinic. Daily self-care activities like exercise, proper nutrition, stress management, and medication adherence determine long-term success. Medical treatments provide tools, but patients must use those tools consistently for optimal benefit.
Realistic Expectations and Hope
Medical experts want patients to understand that while arthritis typically cannot be cured, it can be effectively managed. Most people with arthritis can maintain active, fulfilling lives with appropriate treatment and lifestyle modifications.
Doctors report increasing optimism about arthritis treatment prospects. New medications continue emerging, and our understanding of disease mechanisms improves constantly. Research into regenerative therapies and other innovative approaches offers hope for even better treatments in the future.
Arthritis Statistics Over the Past Century in America
Examining arthritis prevalence and impact over the past 100 years reveals dramatic changes in diagnosis, treatment, and outcomes. This historical perspective helps us understand how far we have come and challenges that remain.
| Time Period | Estimated Prevalence | Major Treatment Approaches | Average Disability Rate | Key Medical Advances |
| 1920s-1930s | Unknown/Not tracked nationally | Rest, aspirin, hot baths, limited physical therapy | Very high, no quantified data | Discovery of aspirin benefits, early physical medicine |
| 1940s-1950s | Approximately 10 million adults | Cortisone introduced, gold salts, improved pain management | Approximately 60% with significant limitations | Discovery of cortisone (1948), first disease-modifying drugs |
| 1960s-1970s | 15-20 million adults | NSAIDs, early joint replacement surgery, physical therapy expansion | Approximately 50% with work limitations | First successful hip replacement (1960), development of NSAIDs |
| 1980s-1990s | 37-40 million adults | Improved DMARDs, better surgical techniques, arthroscopy advances | Approximately 40% with activity limitations | Methotrexate for rheumatoid arthritis, improved imaging technology |
| 2000s-2010s | 52-54 million adults | Biologic medications, minimally invasive surgery, comprehensive care models | Approximately 43% with limitations (but better functional outcomes) | First biologic drugs (1998 onward), treat-to-target strategies |
| 2020-Present | 58+ million adults | Advanced biologics, targeted synthetic DMARDs, precision medicine approaches | Approximately 41% with limitations (improving quality despite higher numbers) | JAK inhibitors, biosimilars increasing access, personalized treatment algorithms |
These statistics reveal several important trends over the past century. The absolute number of people with arthritis has increased substantially, driven primarily by population aging and better diagnostic capabilities. However, the disability rates have improved despite higher prevalence, reflecting advances in treatment and management strategies.
The introduction of biologic medications in the late 1990s and 2000s marked a revolutionary shift in arthritis care. These drugs allow many people with inflammatory arthritis to achieve remission or near-remission, outcomes that were impossible with older treatments.
Is Arthritis Reversible or Chronic? Understanding Disease Progression
One of the most common questions patients ask concerns whether arthritis can be reversed or cured. The answer depends on the type arthritis and how we define “reversal.”
Most Forms Are Chronic but Manageable
The majority of arthritis types are chronic conditions that persist throughout life once they develop. Osteoarthritis cannot be reversed because damaged cartilage does not regenerate naturally. The structural changes in bones and joints remain permanent.
Rheumatoid arthritis and other autoimmune forms of arthritis also represent chronic diseases. While symptoms can be controlled and disease activity suppressed, the underlying immune system dysfunction persists. Stopping medications typically results in symptom return, indicating that the disease remains present even when controlled.
Disease Activity Can Be Controlled
Although most arthritis cannot be cured, modern treatments can suppress disease activity so effectively that many people achieve remission. In this state, they experience minimal or no symptoms and no active inflammation. For practical purposes, their condition becomes manageable rather than disabling.
Inflammatory arthritis types respond particularly well to current medications. Many patients taking biologic drugs or targeted synthetic DMARDs maintain remission for years. They can work, exercise, and participate fully in life without significant limitations from arthritis.
Early Treatment Prevents Progression
While existing joint damage cannot be reversed, treatment can prevent future damage. This makes early intervention crucial. Starting disease-modifying treatments before significant joint destruction occurs preserves joint structure and function.
Studies show that people who begin treatment for rheumatoid arthritis within three to six months of symptom onset have much better long-term outcomes than those who delay treatment. Their joints sustain less damage over time, and they experience fewer complications.
Exceptions: Conditions That May Resolve
Certain arthritis-related conditions can potentially resolve. Reactive arthritis, which develops after some infections, may improve completely once the triggering infection clears. Gout attacks can be prevented entirely through medication and lifestyle changes that control uric acid levels.
Post-traumatic arthritis following injury sometimes stabilizes without progressive worsening, especially if the initial injury heals properly and the joint receives appropriate rehabilitation.
The Importance of Realistic Expectations
Understanding that arthritis is typically chronic helps people develop appropriate expectations and commit to long-term management strategies. This does not mean accepting poor quality of life. Rather, it means recognizing that ongoing treatment and self-care will be necessary.
With proper management, most people with arthritis can lead full, active lives. The condition becomes one aspect of their health to monitor and manage, not a disability that defines their existence.
Lifestyle Factors That Lead to Arthritis Development

While some arthritis risk factors like age and genetics cannot be changed, lifestyle choices significantly influence both the likelihood of developing arthritis and its severity. Understanding these modifiable factors empowers people to take protective action.
Obesity and Excess Body Weight
Excess body weight represents the single most important modifiable risk factor for developing osteoarthritis. The mechanical stress on weight-bearing joints accelerates cartilage breakdown. Obesity also promotes systemic inflammation throughout the body, which can trigger or worsen inflammatory types arthritis.
Research demonstrates that people who are obese face four times the risk of developing knee osteoarthritis compared to those at healthy weights. The risk increases progressively with higher body mass index. Even modest weight gain in young adulthood significantly increases arthritis risk decades later.
Physical Inactivity and Sedentary Behavior
Lack of regular physical activity weakens muscles that support and protect joints. Sedentary people also tend to have less flexible joints and poorer balance, increasing injury risk. Physical inactivity contributes to weight gain, compounding its negative effects on joint health.
Extended periods of sitting or lying down allow joints to stiffen. Movement keeps synovial fluid circulating, which nourishes cartilage and removes waste products. Without regular movement, joint health deteriorates even in the absence of excess weight.
Poor Dietary Patterns
Diets high in processed foods, red meat, and added sugars promote inflammation throughout the body. This inflammatory state damages joints over time and may trigger autoimmune responses in susceptible individuals. The standard American diet, unfortunately, exemplifies these harmful patterns.
Inadequate intake of nutrients important for bone and joint health also contributes to arthritis risk. Deficiencies in vitamin D, calcium, and omega-3 fatty acids compromise joint integrity and repair mechanisms. Many Americans consume insufficient amounts of these protective nutrients.
Smoking and Tobacco Use
Smoking dramatically increases the risk of developing rheumatoid arthritis, particularly in people with genetic susceptibility. The chemicals in tobacco smoke trigger inflammatory responses and may activate dormant autoimmune tendencies. Smokers who develop rheumatoid arthritis typically experience more severe disease and respond less well to treatment.
Smoking also impairs healing and reduces blood flow to joints. This interferes with the body’s natural repair processes, allowing damage to accumulate more rapidly. The negative effects persist for years even after quitting, though stopping provides benefits at any age.
Occupational and Recreational Joint Stress
Jobs or hobbies requiring repetitive motions stress particular joints over time. Occupations involving frequent kneeling, squatting, or lifting increase knee and hip arthritis risk. Assembly line workers, construction workers, and agricultural laborers face elevated rates of osteoarthritis in heavily used joints.
Recreational activities also impact joint health. While exercise provides benefits, certain high-impact sports or activities with repetitive joint stress may increase arthritis risk, especially if proper technique and equipment are not used. Previous sports injuries significantly elevate future arthritis risk in affected joints.
Inadequate Injury Treatment and Recovery
Failing to properly treat and rehabilitate joint injuries sets the stage for post-traumatic arthritis. Ligament tears, cartilage damage, and fractures involving joint surfaces require appropriate medical care and complete rehabilitation. Returning to full activity too quickly before healing completes increases the likelihood of progressive joint damage.
Many people underestimate minor joint injuries, dismissing persistent pain or limited mobility as temporary. This delay in seeking treatment allows problems to worsen and increases long-term arthritis risk substantially.
Daily Habits That Reduce Joint Problems and Protect Against Arthritis

Adopting protective habits significantly reduces arthritis risk and helps manage existing joint problems more effectively. These daily practices work cumulatively over time to preserve joint health and function.
Maintain a Healthy Weight
Keeping body weight within the healthy range provides the single greatest protection against osteoarthritis. Even modest weight loss produces meaningful benefits. Losing 5 to 10 percent of body weight reduces knee pain and improves function in people who are overweight.
Weight management requires consistent attention to both diet and activity. Focusing on whole foods, controlling portion sizes, and limiting processed items creates sustainable eating patterns. Combining dietary changes with regular physical activity produces the best long-term results.
Exercise Regularly with Joint-Friendly Activities
Regular exercise strengthens muscles that support joints, maintains flexibility, and promotes overall health. The key lies in choosing activities appropriate for your current condition and gradually progressing as fitness improves.
Low-impact aerobic exercises provide cardiovascular benefits without excessive joint stress. Swimming, water aerobics, cycling, and walking represent excellent choices. Aim for at least 150 minutes of moderate activity weekly, spread across most days.
Strength training builds muscle mass that cushions and stabilizes joints. Focus on all major muscle groups, performing exercises two to three times weekly. Start with light resistance and proper form before increasing weight.
Protect Joints During Activities
Using proper body mechanics during daily tasks reduces unnecessary joint stress. When lifting, bend at the knees rather than the waist and keep heavy objects close to your body. Use both hands to distribute weight when carrying items.
Take regular breaks during repetitive activities to rest joints and change positions. Alternate between different tasks rather than performing the same motion for extended periods. Use assistive devices like jar openers, reaching tools, or ergonomic handles when they reduce joint strain.
Eat an Anti-Inflammatory Diet
Dietary patterns emphasizing anti-inflammatory foods help reduce systemic inflammation that damages joints. Base meals around vegetables, fruits, whole grains, legumes, nuts, and fatty fish. These foods provide nutrients and compounds that combat inflammation.
Minimize consumption of foods that promote inflammation. Limit red meat, processed meats, refined carbohydrates, and foods high in added sugars. Reduce or eliminate trans fats found in some processed foods.
Specific foods show particular promise for joint health. Fatty fish like salmon, mackerel, and sardines provide omega-3 fatty acids. Colorful fruits and vegetables supply antioxidants. Green tea contains compounds with anti-inflammatory properties. Turmeric and ginger possess natural anti-inflammatory effects.
Stay Hydrated
Adequate hydration helps maintain the cushioning properties of cartilage. Water makes up much of the cartilage structure, and proper hydration keeps this tissue functioning optimally. Aim for eight glasses of water daily, adjusting for activity level and climate.
Prioritize Quality Sleep
Good sleep supports tissue repair and reduces inflammation throughout the body. Poor sleep increases pain sensitivity and inflammatory markers. Adults should aim for seven to nine hours of quality sleep nightly.
Establish consistent sleep schedules and create a relaxing bedtime routine. Keep the bedroom cool, dark, and quiet. Address sleep problems promptly, as chronic sleep deprivation worsens arthritis symptoms and overall health.
Manage Stress Effectively
Chronic stress increases inflammation and may trigger flares in inflammatory arthritis. Stress also amplifies pain perception, making symptoms feel worse. Developing healthy stress management techniques protects both mental and physical health.
Effective stress reduction methods include meditation, deep breathing exercises, yoga, and spending time in nature. Regular social connections and maintaining hobbies also buffer against stress effects. Consider professional counseling if stress becomes overwhelming.
Avoid Smoking and Limit Alcohol
Quitting smoking provides immediate and long-term benefits for joint health. The inflammatory effects begin reversing within weeks of stopping. Resources like counseling, medications, and support groups improve success rates significantly.
Limit alcohol consumption to moderate levels or avoid it entirely. Excessive alcohol intake promotes inflammation and interferes with medication effectiveness for arthritis treatment.
Get Regular Health Screenings
Routine medical checkups allow early detection of arthritis and related conditions. Discuss any persistent joint pain, stiffness, or swelling with your healthcare provider. Blood tests can identify inflammatory markers or conditions that increase arthritis risk.
People with family history of arthritis or other risk factors may benefit from more frequent monitoring. Early detection enables earlier treatment, which produces better long-term outcomes.
Taking Action Against America’s Arthritis Crisis

Arthritis represents one of the most significant health challenges facing Americans today, affecting more than 58 million adults and imposing enormous personal and economic costs. The disease impacts people across all age groups, though risk increases substantially after age 45. The burden extends beyond physical symptoms to affect mental health, employment, relationships, and overall quality of life.
Understanding arthritis empowers individuals to take protective action. While some risk factors cannot be changed, many lifestyle modifications significantly reduce arthritis risk or slow its progression. Maintaining healthy weight, exercising regularly, eating an anti-inflammatory diet, protecting joints from injury, and avoiding tobacco use all contribute to better joint health.
For those already living with arthritis, effective treatments now exist that can dramatically improve symptoms and function. Modern medications, particularly for inflammatory types arthritis, can suppress disease activity and prevent progressive joint damage. Physical therapy, appropriate exercise, and comprehensive self-management strategies enhance treatment effectiveness.
The key to success lies in early action. Whether preventing arthritis or managing existing disease, starting protective measures and treatments early produces the best outcomes. Do not dismiss persistent joint symptoms as normal aging or minor problems. Seek medical evaluation promptly to begin appropriate interventions before extensive damage occurs.
Most importantly, recognize that arthritis does not have to control your life. With proper management combining medical treatment, lifestyle modifications, and consistent self-care, most people with arthritis can maintain active, fulfilling lives. The condition becomes manageable rather than disabling, allowing you to continue pursuing the activities and relationships that matter most.