Alzheimer’s Disease: Understanding America’s Growing Health Crisis
Alzheimer disease stands as one of the most devastating neurological conditions facing the United States today. This progressive brain disorder affects millions of Americans and their families. The disease destroys memory and thinking skills over time. Eventually, it takes away the ability to carry out simple tasks.
As our population ages, more people face this challenging diagnosis each year. Understanding this condition becomes critical for families across the nation. Knowledge about symptoms, prevention, and treatment options can make a real difference.
Why Alzheimer’s Disease Poses a Major Threat to US Health
Alzheimer disease represents a critical public health challenge in the United States. The numbers tell a sobering story about this condition’s impact on our society. More than six million Americans currently live with this brain disease. That number continues to grow each year.
The financial burden is staggering. Americans spend hundreds of billions of dollars annually on care for people with dementia. These costs affect families, healthcare systems, and the broader economy. Many families face financial hardship as they navigate long-term care needs.
Beyond money, the human cost proves immeasurable. Caregivers experience tremendous stress and emotional strain. The disease affects not just patients but entire families. Communities feel the impact as more people lose their ability to work and participate in daily life.
Healthcare systems struggle to meet growing demand. Hospitals and care facilities need more specialized resources. Trained professionals who understand dementia care remain in short supply. This gap between need and available support continues to widen.
Critical Impact: Alzheimer disease now ranks as the sixth leading cause of death in the United States. It is the only condition among the top ten causes of death that cannot be prevented, cured, or even slowed.
What is Alzheimer’s Disease: A Clear Definition
Alzheimer disease is a progressive brain disorder that damages and destroys brain cells over time. This condition represents the most common form of dementia. The disease causes continuous decline in thinking, behavior, and social skills.
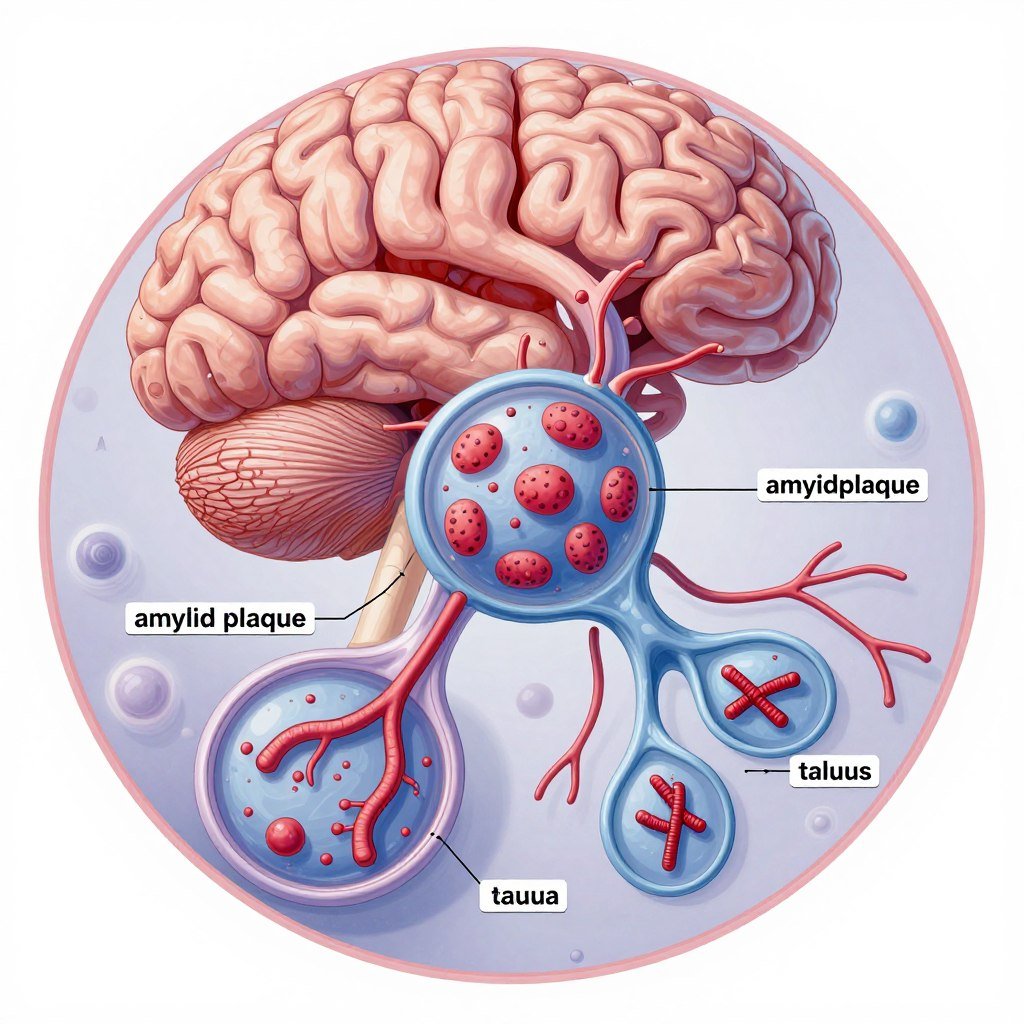
Inside the brain, the disease creates specific changes. Abnormal protein deposits form between nerve cells. These deposits, called plaques, contain a protein fragment called amyloid. Another protein, called tau, creates tangles inside cells. These tangles and plaques interfere with how brain cells communicate.
How the Disease Affects the Brain
Brain cells die as the disease progresses. The brain actually shrinks in size. Areas important for memory and thinking suffer the most damage. The hippocampus, which forms new memories, shows damage early in the disease.
Connections between neurons break down. This disruption prevents normal brain function. Eventually, widespread brain damage makes it impossible for the person to live independently. The loss of nerve cells and their connections causes the visible symptoms.
Scientists classify Alzheimer disease as a type of dementia. Dementia describes a group of symptoms affecting memory, thinking, and social abilities. While all Alzheimer disease is dementia, not all dementia comes from Alzheimer disease. Other conditions can cause similar symptoms through different brain changes.
Key Distinction: Alzheimer disease differs from normal aging. Everyone experiences some memory changes with age. However, Alzheimer disease causes severe memory problems that interfere with daily life. The condition is not a normal part of getting older.
Age Groups Most Affected by Alzheimer’s Disease
Age serves as the greatest risk factor for developing Alzheimer disease. The condition primarily affects older adults. However, the disease can appear in people at different life stages.

Older Adults Face the Highest Risk
Most people with Alzheimer disease are age sixty-five or older. After this age, the risk doubles approximately every five years. By age eighty-five, the risk reaches nearly one-third of the population. This age group represents the largest number of cases in the United States.
The national institute aging reports that people in their eighties and nineties show the highest prevalence. As Americans live longer, more people reach ages where risk increases substantially. This demographic shift explains why total case numbers keep rising.
Early-Onset Cases in Younger Adults
Some people develop symptoms before age sixty-five. Experts call this early-onset Alzheimer disease. While less common, it affects approximately two hundred thousand Americans. These younger patients face unique challenges in diagnosis and care.
People in their forties and fifties can develop this condition. Early-onset cases often have genetic factors. Families with a history of early symptoms may carry specific gene mutations. These cases progress through similar stages but affect people during their working years.
| Age Group | Risk Level | Estimated Prevalence | Key Characteristics |
| Under 65 | Low | Less than 5% | Early-onset cases, often genetic factors |
| 65-74 | Moderate | 5-10% | Initial risk increase, early symptoms |
| 75-84 | High | 15-20% | Significant risk elevation, common diagnosis age |
| 85+ | Very High | 30-50% | Highest risk group, multiple contributing factors |
Women show slightly higher rates than men across all age groups. Scientists continue studying whether biological differences or longer life expectancy explains this pattern. Regardless of gender, advancing age remains the most significant factor in disease development.
How Alzheimer’s Has Become Overwhelming in the United States
The United States faces an unprecedented crisis as Alzheimer disease cases multiply. The situation has grown increasingly difficult to manage. Multiple factors contribute to this overwhelming challenge facing families and healthcare systems.

Rising Numbers Create Care Shortages
More people develop the disease each year than ever before. The aging baby boomer generation now reaches prime risk ages. This demographic wave creates unprecedented demand for specialized care. Facilities and healthcare providers cannot keep pace with growing needs.
Families struggle to find qualified caregivers. Long waiting lists exist for memory care facilities. Home care workers with dementia training remain scarce. This shortage means many families must provide care themselves without proper training or support.
Financial Strain on Families and Systems
The cost of care reaches catastrophic levels for many families. Average lifetime expenses for one patient can exceed hundreds of thousands of dollars. Insurance coverage often proves inadequate. Medicare does not cover most long-term care services that people with dementia require.
Out-of-pocket expenses devastate family finances. Many caregivers must leave their jobs to provide full-time care. This loss of income compounds already high medical costs. Families deplete savings and retirement funds trying to provide proper care.
Healthcare System Challenges
- Insufficient specialized memory care units
- Shortage of trained dementia care professionals
- Long wait times for diagnostic services
- Limited access to clinical trials and new treatments
- Inadequate support services for families
Family Burden Factors
- Twenty-four hour supervision requirements
- Emotional toll of watching cognitive decline
- Physical exhaustion from constant caregiving
- Social isolation as care demands increase
- Difficulty balancing work and care responsibilities
Emotional and Social Consequences
Caregivers face severe emotional stress. Depression and anxiety become common among those caring for loved ones with the disease. The constant demands leave little time for self-care. Many caregivers experience their own health problems from prolonged stress.
Social connections deteriorate as the disease progresses. Both patients and caregivers become increasingly isolated. Friends and extended family may withdraw, unsure how to help. This isolation intensifies the burden on primary caregivers.
The disease affects entire communities. Workplaces lose experienced employees who become caregivers. Productivity drops as workers juggle job responsibilities with care duties. The broader economic impact extends far beyond individual families.
Alzheimer’s Disease Statistics Over 100 Years in the United States
The history of Alzheimer disease recognition and prevalence spans more than a century. Understanding how case numbers have changed reveals the growing scale of this health crisis. Statistical tracking has improved dramatically over time.
Early recognition of the disease began in the nineteen hundreds. However, systematic tracking did not start until much later. Medical understanding and diagnostic capabilities have evolved significantly. This improvement allows better case identification and data collection.
| Decade | Estimated Cases | Death Rate per 100,000 | Key Developments |
| 1920s | Under 100,000 | Not tracked | Disease first identified, rare diagnosis |
| 1930s | Under 150,000 | Not tracked | Limited medical awareness, often misdiagnosed |
| 1940s | Under 200,000 | Not tracked | World War II impacts research priorities |
| 1950s | 300,000 | 5.2 | Improved diagnostic techniques emerge |
| 1960s | 500,000 | 6.8 | Better recognition of dementia symptoms |
| 1970s | 1,000,000 | 8.1 | National Institute Aging established |
| 1980s | 2,000,000 | 10.5 | Alzheimer’s Association founded, increased awareness |
| 1990s | 3,000,000 | 13.2 | First medications approved for treatment |
| 2000s | 4,500,000 | 20.8 | Advanced brain imaging technologies available |
| 2010s | 5,800,000 | 29.4 | Biomarker research advances significantly |
| 2020s | 6,700,000 | 32.1 | New treatment approaches in clinical trials |
The dramatic increase in cases reflects several factors. Population aging contributes significantly to rising numbers. Better diagnostic tools identify more cases. Increased awareness leads to more people seeking evaluation. Longer life expectancy means more people reach ages of highest risk.
Death rates from Alzheimer disease have climbed steeply. The condition now ranks among leading causes of death in the United States. Unlike other major causes of death, rates continue to rise rather than decline. This trend underscores the urgent need for effective prevention and treatment strategies.
How to Prevent Alzheimer’s Disease
While no guaranteed prevention exists, research shows certain actions may reduce risk. Scientists have identified several lifestyle factors that appear protective. Implementing these strategies may delay onset or reduce severity of symptoms.

Physical Activity and Exercise
Regular physical activity shows strong protective effects. Exercise improves blood flow to the brain. It supports the growth of new nerve cells. Activities that elevate heart rate provide the most benefit.
Experts recommend at least one hundred fifty minutes of moderate exercise weekly. Walking, swimming, and cycling all offer brain health benefits. Even modest activity levels help compared to sedentary lifestyles. Starting an exercise routine at any age provides value.
Mental Stimulation and Learning
Keeping the brain active may build cognitive reserve. This reserve might help the brain compensate for damage. Learning new skills creates additional neural connections. Mental challenge throughout life appears protective.
Brain-Healthy Activities
- Learning new languages or instruments
- Solving puzzles and playing strategic games
- Reading and engaging with complex material
- Taking classes and pursuing education
- Engaging in creative hobbies and arts
- Using technology and learning new skills
Social Engagement
- Maintaining strong social connections
- Participating in community activities
- Volunteering and helping others
- Joining clubs and interest groups
- Regular interaction with family and friends
- Staying involved in meaningful activities
Heart-Healthy Diet
What benefits the heart also helps the brain. A Mediterranean-style diet shows particular promise. This eating pattern emphasizes vegetables, fruits, whole grains, and healthy fats. Fish provides omega-three fatty acids important for brain health.
Limiting processed foods and added sugars supports cognitive health. Excessive alcohol consumption increases risk. Maintaining healthy blood pressure and cholesterol levels protects brain cells. These dietary choices impact both heart disease and dementia risk.
Managing Health Conditions
Controlling certain medical conditions reduces risk. Diabetes management proves particularly important. High blood pressure damages blood vessels in the brain. Treating these conditions protects cognitive function.
Head injuries increase Alzheimer risk later in life. Wearing seatbelts and helmets prevents traumatic brain injury. Sleep quality affects brain health significantly. Treating sleep disorders may offer protective benefits.
Is Treatment Really Helpful: What Doctors Are Saying
Current treatments for Alzheimer disease cannot cure or stop the condition. However, available options can help manage symptoms. Medical professionals emphasize realistic expectations while remaining hopeful about emerging therapies.

Available Medication Options
Several medications can temporarily slow symptom progression. Cholinesterase inhibitors help with memory and thinking problems. These drugs work by increasing chemical messengers in the brain. They provide modest benefit for some people in early to middle stages.
Another medication type regulates glutamate activity in the brain. This approach may help with learning and memory. Doctors often prescribe these medications in moderate to severe stages. Response varies significantly between individuals.
Recently approved treatments target amyloid plaques directly. These newer drugs represent the first disease-modifying therapies. Early results show they can slow cognitive decline in some patients. However, they come with significant side effects and high costs.
What Neurologists Emphasize
Brain specialists stress early diagnosis importance. Starting treatment during mild symptoms may provide better outcomes. Regular monitoring allows doctors to adjust approaches as the disease progresses. Comprehensive care plans address multiple aspects of the condition.
“Current treatments offer meaningful benefits for many patients, especially when started early. While we cannot yet cure Alzheimer disease, we can improve quality of life and slow progression. The key is early detection and a comprehensive treatment approach that includes both medication and lifestyle interventions.”
Doctors emphasize that medication represents only part of treatment. Managing other health conditions matters greatly. Depression and anxiety often accompany dementia. Treating these conditions improves overall function and quality of life.
Non-Drug Approaches
Behavioral interventions help manage symptoms. Structured routines reduce confusion and anxiety. Environmental modifications create safer living spaces. These approaches work alongside medication to support daily functioning.
Medical Interventions
- Cholinesterase inhibitor medications
- Glutamate regulators
- Amyloid-targeting therapies
- Management of related conditions
Therapeutic Support
- Cognitive stimulation therapy
- Occupational therapy services
- Speech and language therapy
- Physical therapy programs
Lifestyle Modifications
- Structured daily routines
- Environmental safety measures
- Social engagement activities
- Caregiver education and support
Clinical trials continue testing new approaches. Researchers investigate treatments targeting different aspects of brain changes. Some trials examine prevention strategies in high-risk individuals. Participation in research contributes to future treatment development.
Realistic Expectations
Medical experts encourage hope balanced with realism. Current treatments provide modest benefits rather than dramatic improvement. The goal focuses on maintaining function and quality of life as long as possible. Family education and support services prove as important as medication.
Doctors stress the importance of planning. Legal and financial decisions should happen while the person can participate. Advance care planning ensures wishes are known and respected. These conversations, though difficult, provide clarity for families.
Is Alzheimer’s Disease Reversible or Chronic
Alzheimer disease is a chronic, progressive condition. Currently, no cure exists that can reverse the brain damage. Once symptoms appear, the disease continues to advance over time. Understanding this reality helps families plan appropriately.
The Progressive Nature of the Disease
Brain cells continue to die throughout the disease course. The damage spreads to additional brain areas over time. Early stages affect memory formation primarily. Later stages impact all cognitive functions and physical abilities.
Average survival after diagnosis ranges from four to eight years. However, some people live twenty years or more with the condition. Progression rate varies significantly between individuals. Multiple factors influence how quickly symptoms worsen.
Why Reversal Remains Impossible
Dead neurons cannot regenerate in the adult brain. The connections between nerve cells, once destroyed, do not reform. Accumulated plaques and tangles cause permanent structural changes. Current medical science cannot repair this extensive brain damage.
Research continues seeking ways to slow or stop progression. Some experimental treatments show promise in early trials. However, reversing existing damage remains beyond current capabilities. Prevention and early intervention offer the best hope for reducing disease impact.
Important Note: Be cautious of claims promising to reverse or cure Alzheimer disease. No legitimate treatment can currently reverse this condition. Anyone offering guaranteed cures likely promotes unproven and potentially dangerous therapies.
Living with a Chronic Condition
Accepting the chronic nature helps families adjust expectations. Focus shifts to maintaining quality of life at each stage. Support systems become increasingly important over time. Planning for long-term care needs allows better preparation.
Despite being irreversible, people can live meaningful lives with support. Early stages allow continued participation in valued activities. Proper care management helps people maintain dignity and comfort. Families find ways to adapt and create positive experiences.
Lifestyle Factors That Lead to Alzheimer’s Disease
Certain lifestyle choices appear to increase risk of developing Alzheimer disease. While genes play a role, controllable factors significantly impact risk. Understanding these connections empowers people to make brain-healthy choices.

Physical Inactivity
Sedentary lifestyles correlate with higher dementia risk. Lack of exercise reduces blood flow to the brain. Physical inactivity contributes to conditions like diabetes and heart disease. These conditions further increase Alzheimer risk.
People who remain inactive throughout life show greater cognitive decline. The brain requires adequate blood supply to function properly. Exercise promotes the growth of new blood vessels in the brain. Regular movement helps clear harmful proteins that accumulate in brain tissue.
Poor Diet Quality
Diets high in saturated fats and processed foods increase risk. These eating patterns promote inflammation throughout the body. Inflammation affects brain health negatively. Excessive sugar consumption links to cognitive decline.
Vitamin deficiencies may contribute to brain changes. Inadequate intake of B vitamins shows particular concern. Diets lacking omega-three fatty acids miss important brain-protective nutrients. Poor nutrition affects both general health and brain function.
Social Isolation
Limited social interaction appears harmful to brain health. Loneliness and isolation increase dementia risk substantially. Social engagement stimulates multiple brain areas simultaneously. Meaningful relationships provide cognitive benefits beyond simple interaction.
People who maintain strong social networks show better cognitive resilience. Social activities require communication, memory, and complex thinking. These mental exercises help maintain brain function. Isolation removes these beneficial stimulation opportunities.
Risk-Increasing Factors
- Chronic physical inactivity and sedentary behavior
- Poor diet quality and nutritional deficiencies
- Social isolation and limited engagement
- Chronic stress and inadequate stress management
- Poor sleep quality and untreated sleep disorders
- Smoking and excessive alcohol consumption
- Uncontrolled cardiovascular risk factors
- Lack of mental stimulation and learning
Additional Contributing Factors
- Chronic inflammation from various sources
- Environmental toxin exposure
- History of traumatic brain injuries
- Unmanaged chronic health conditions
- Prolonged medication use affecting cognition
- Lack of purpose and meaningful activities
- Poor air quality and pollution exposure
- Inadequate sunlight and vitamin D deficiency
Substance Use
Smoking damages blood vessels throughout the body and brain. Tobacco use significantly increases dementia risk. Even secondhand smoke exposure shows negative effects. Quitting smoking reduces risk at any age.
Heavy alcohol consumption causes direct brain damage. Excessive drinking over years shrinks brain tissue. While moderate consumption may not harm, heavy use clearly increases risk. Substance abuse creates multiple pathways to cognitive impairment.
Stress and Mental Health
Chronic stress appears linked to higher dementia risk. Stress hormones may damage brain areas important for memory. Untreated depression and anxiety show associations with later cognitive decline. Mental health management supports brain health.
Sleep problems contribute to risk in multiple ways. Poor sleep prevents the brain from clearing harmful proteins. Sleep apnea reduces oxygen supply to the brain. Addressing sleep issues may provide protective benefits.
Habits That Support Brain Health
Adopting specific daily habits can promote long-term brain health. These practices support cognitive function and may reduce Alzheimer risk. Starting these habits at any age provides benefit.

Regular Physical Exercise
Consistent aerobic activity provides powerful brain benefits. Walking thirty minutes daily offers substantial protection. Exercise does not need to be intense to help. Finding enjoyable activities increases adherence to exercise routines.
Strength training also supports cognitive health. Balance exercises prevent falls that could cause head injury. Combining different exercise types provides comprehensive benefits. Movement throughout the day matters more than single workout sessions.
Nutritious Eating Patterns
Following a Mediterranean-style diet shows strong brain-protective effects. This approach emphasizes whole, unprocessed foods. Colorful vegetables and fruits provide antioxidants that protect brain cells. Healthy fats from fish, nuts, and olive oil support brain structure.
Physical Health Habits
- Daily aerobic exercise for thirty minutes
- Strength training twice weekly
- Adequate hydration throughout the day
- Seven to eight hours quality sleep nightly
Mental Stimulation Habits
- Learning new skills and hobbies
- Reading challenging material regularly
- Solving puzzles and strategic games
- Engaging in creative activities
Social Connection Habits
- Regular contact with friends and family
- Participating in group activities
- Volunteering in the community
- Maintaining meaningful relationships
Continuous Learning
Challenging the brain with new information builds cognitive reserve. Taking classes keeps the mind active and engaged. Learning languages provides particularly strong benefits. Any new skill acquisition creates beneficial neural connections.
Reading regularly exercises multiple cognitive functions. Complex material requires focus, comprehension, and memory. Discussing what you read adds social and analytical components. These combined activities strengthen various brain areas.
Quality Sleep
Prioritizing good sleep supports brain health significantly. During sleep, the brain clears waste products including harmful proteins. Consistent sleep schedules help regulate this cleaning process. Creating optimal sleep environments improves rest quality.
Treating sleep disorders proves important for brain protection. Sleep apnea requires medical intervention. Insomnia management may include behavioral approaches. Good sleep hygiene habits benefit everyone regardless of age.
Stress Management
Developing healthy stress coping mechanisms protects the brain. Meditation and mindfulness practices show measurable brain benefits. These techniques reduce harmful stress hormone levels. Regular practice improves emotional regulation and cognitive function.
Engaging in enjoyable activities provides stress relief. Hobbies offer mental breaks from daily pressures. Time in nature shows particular stress-reducing benefits. Building relaxation practices into daily routines supports long-term brain health.
Social Engagement
Maintaining active social lives exercises cognitive function. Conversations require memory, attention, and complex thinking. Group activities provide structure and purpose. Meaningful relationships offer emotional support that benefits brain health.
Volunteering combines social interaction with purposeful activity. Helping others provides psychological benefits beyond social connection. Community involvement keeps people engaged with the world. These activities stimulate multiple aspects of brain function simultaneously.
Taking Action for Brain Health
Alzheimer disease presents a significant challenge to individuals, families, and society. Understanding this condition empowers people to make informed decisions. Knowledge about risk factors, prevention strategies, and available treatments provides hope despite the disease’s serious nature.

The statistics reveal a growing crisis requiring urgent attention. However, research continues advancing our understanding. New treatments emerge from ongoing clinical trials. Every day brings us closer to more effective interventions.
Individual actions matter significantly. Lifestyle modifications can reduce personal risk. Brain-healthy habits benefit overall well-being beyond dementia prevention. Starting these practices today protects cognitive function for years to come.
For those facing diagnosis, comprehensive support exists. Medical treatments combined with behavioral approaches improve quality of life. Families need not navigate this journey alone. Resources and communities offer guidance and assistance throughout all stages.
Early detection allows better planning and treatment outcomes. Regular health checkups should include cognitive assessments. Speaking with healthcare providers about memory concerns enables timely intervention. Proactive approaches provide the best opportunity for maintaining function and independence.
The fight against Alzheimer disease requires both individual and collective action. Supporting research advances our knowledge and treatment capabilities. Advocating for better healthcare policies ensures resources reach those who need them. Together, we work toward a future where this disease no longer devastates families and communities.