Sleep Disorders in the USA: A Critical Health Crisis
Sleep disorders have become a silent epidemic in the United States. Millions of Americans struggle every night to get quality rest. The consequences extend far beyond feeling tired.
These conditions affect physical health, mental well-being, and daily performance. They impact relationships, work productivity, and overall quality of life.
Understanding sleep disorders is the first step toward reclaiming restful nights. This comprehensive guide explores everything you need to know about these conditions affecting American health.
Why Sleep Disorders Are a Major Threat to US Health
Sleep disorders represent one of the most significant yet overlooked health challenges facing Americans today. The American Academy Sleep Medicine reports that these conditions affect between 50 and 70 million adults nationwide.
The impact on public health extends beyond individual suffering. Sleep disorders contribute to serious medical conditions including heart disease, diabetes, and stroke. They compromise immune function and accelerate aging processes.
Economic costs are staggering. Lost productivity, workplace accidents, and healthcare expenses related to sleep disorders exceed $400 billion annually in the United States.
Motor vehicle accidents caused by drowsy driving claim thousands of lives each year. The National Highway Traffic Safety Administration estimates that fatigue contributes to 100,000 crashes annually.
Critical fact: Untreated sleep apnea increases the risk of high blood pressure by 300% and doubles the risk of heart attack and stroke.
Mental health connections are equally concerning. Sleep disorders and depression create a cyclical relationship where each condition worsens the other. Anxiety disorders frequently coexist with insomnia and other sleep disturbances.
What Are Sleep Disorders? Complete Definition
Sleep disorders are medical conditions that disrupt normal sleep patterns and prevent restorative rest. These disorders interfere with the ability to fall asleep, stay asleep, or achieve quality sleep.
The American Academy Sleep Medicine recognizes over 80 distinct sleep disorders. They fall into several major categories based on symptoms and underlying causes.
Primary Categories
- Insomnia – difficulty falling or staying asleep
- Sleep apnea – breathing interruptions during sleep
- Circadian rhythm disorders – misaligned sleep-wake cycles
- Parasomnias – abnormal movements or behaviors during sleep
- Hypersomnia – excessive daytime sleepiness
- Movement disorders – restless legs syndrome and periodic limb movements
Sleep medicine specialists use comprehensive criteria to diagnose these conditions. Diagnosis typically requires detailed sleep history, physical examination, and often overnight sleep studies.
Common symptoms that indicate a sleep disorder include chronic difficulty falling asleep, frequent nighttime awakenings, loud snoring with breathing pauses, excessive daytime sleepiness, and unusual movements or behaviors during sleep.
Medical Definition: According to the Academy Sleep Medicine, a sleep disorder is diagnosed when sleep disturbances occur at least three times per week for a minimum of three months and cause significant distress or impairment in daily functioning.
These conditions differ from occasional poor sleep. Everyone experiences sleepless nights occasionally. Sleep disorders persist over time and resist typical solutions like earlier bedtimes or relaxation techniques.
Age Groups Most Affected by Sleep Disorders USA
Sleep disorders impact Americans across all age groups, but certain populations face higher risks. Understanding these patterns helps identify vulnerable groups and target prevention efforts.

Adults Aged 40-60: Peak Vulnerability
Middle-aged adults experience the highest rates of sleep disorders. Studies show that 60% of adults in this age group report regular sleep problems.
Sleep apnea becomes significantly more common after age 40. Risk factors including weight gain and hormonal changes contribute to increased prevalence.
Work stress, caregiving responsibilities, and health conditions converge during these years. Many adults juggle career demands with caring for aging parents and supporting children.
Seniors Over 65: Complex Sleep Challenges
Older adults face unique sleep challenges. Nearly 50% of seniors report chronic insomnia symptoms.
Age-related changes in circadian rhythm cause earlier sleep and wake times. Seniors often experience lighter, more fragmented sleep with frequent nighttime awakenings.
Multiple medications common in this age group can interfere with sleep quality. Chronic health conditions including arthritis, heart disease, and respiratory problems disrupt rest.
Young Adults 18-39: The Overlooked Population
Younger adults increasingly struggle with sleep disorders. Technology use, irregular schedules, and academic or career pressures take a toll.
This group shows rising rates of insomnia linked to anxiety and depression. Social media use before bed disrupts natural sleep-wake cycles.
Shift work is common among young adults. Irregular schedules conflict with biological circadian rhythm needs.
| Age Group | Most Common Disorder | Prevalence Rate | Primary Risk Factors |
| 18-29 years | Insomnia | 25-30% | Technology use, irregular schedules |
| 30-39 years | Insomnia, Early Sleep Apnea | 35-40% | Stress, young children |
| 40-49 years | Sleep Apnea | 45-50% | Weight gain, hormonal changes |
| 50-59 years | Sleep Apnea, Restless Legs | 55-60% | Chronic conditions, menopause |
| 60+ years | Insomnia, Sleep Maintenance | 50-55% | Multiple medications, health conditions |
Gender Differences in Sleep Disorders
Women experience higher rates of insomnia throughout most of their lives. Hormonal fluctuations during menstruation, pregnancy, and menopause affect sleep patterns.
Men show higher prevalence of sleep apnea, particularly obstructive sleep apnea. Anatomical differences in airway structure contribute to this disparity.
How Sleep Disorders Become Stressful and Out of Control
Sleep disorders create cascading effects that spiral beyond nighttime struggles. The progression from occasional sleep problems to chronic, life-altering conditions follows predictable patterns.

The Downward Cycle of Sleep Deprivation
Poor sleep triggers anxiety about sleep itself. This performance anxiety makes falling asleep even harder. The bed becomes associated with frustration rather than rest.
Daytime fatigue leads to poor decisions. People consume excessive caffeine to stay alert. This creates a vicious cycle where stimulants prevent nighttime sleep.
Relationships suffer when irritability and mood changes become constant. Partners may sleep separately due to snoring or restless movements. This creates emotional distance.
Professional and Financial Consequences
Work performance deteriorates with chronic sleep deprivation. Concentration, memory, and decision-making abilities decline. Errors increase and productivity drops.
Many adults with untreated sleep disorders face career setbacks. Some lose jobs due to absenteeism or performance issues. Others cannot advance due to reduced cognitive function.
Medical expenses accumulate. Treatment for sleep disorders and related health conditions creates financial stress. Insurance may not cover all necessary care.
Physical Health Spiral
- Weight gain from hormonal disruption
- Increased blood pressure
- Weakened immune system
- Higher diabetes risk
- Chronic pain conditions worsen
- Accelerated aging
Mental Health Impact
- Depression symptoms emerge or worsen
- Anxiety levels increase
- Emotional regulation difficulties
- Memory problems develop
- Social withdrawal
- Reduced quality of life
Why Problems Escalate in the USA
American culture contributes to worsening sleep disorders. The “sleep when you’re dead” mentality minimizes the importance of rest. Many people view sleep as optional or lazy.
Healthcare system challenges delay diagnosis and treatment. Primary care physicians often have limited time to address sleep concerns. Referrals to sleep specialists can take months.
Financial barriers prevent many from seeking help. Sleep studies are expensive. Continuous positive airway pressure devices and other treatments require significant investment.
Work schedules in the USA often conflict with biological sleep needs. Long commutes, overtime demands, and shift work disrupt natural circadian rhythm patterns.
Warning signs your sleep disorder is escalating: Missing work regularly, relying on alcohol or medications to sleep, experiencing microsleeps during the day, or having frequent accidents or near-misses.
How to Prevent Sleep Disorders: Evidence-Based Strategies
Prevention strategies can significantly reduce sleep disorder risk. Many conditions develop gradually and respond well to early intervention.

Establish Strong Sleep Hygiene
Sleep hygiene forms the foundation of disorder prevention. These habits create optimal conditions for restorative sleep.
Maintain consistent sleep and wake times every day. Your body’s circadian rhythm thrives on regularity. Even weekend schedule changes disrupt this biological clock.
Create a bedroom environment dedicated to sleep. Keep the room cool, dark, and quiet. Remove televisions, computers, and work materials from the sleeping space.
- Set bedroom temperature between 60-67°F for optimal sleep
- Use blackout curtains or eye masks to block light
- Invest in comfortable mattress and pillows
- Use white noise machines if needed to mask disruptive sounds
- Reserve the bed exclusively for sleep and intimacy
Time Your Activities Strategically
When you eat, exercise, and consume substances significantly impacts sleep quality. Strategic timing prevents common sleep disruptions.
Avoid caffeine after 2 PM. This stimulant remains in your system for six to eight hours. Even afternoon coffee can interfere with nighttime sleep.
Stop eating large meals three hours before bed. Digestion can interfere with sleep onset. Light snacks are acceptable if needed.
Exercise regularly but finish vigorous workouts at least four hours before bedtime. Physical activity promotes better sleep but creates temporary alertness.
Manage Stress and Mental Health
Psychological factors play crucial roles in sleep disorder development. Addressing stress and mental health protects sleep quality.
Practice relaxation techniques daily. Deep breathing, progressive muscle relaxation, and meditation reduce anxiety that interferes with sleep.
Establish a wind-down routine starting one hour before bed. This signals your body that sleep time approaches. Activities might include reading, gentle stretching, or listening to calm music.
Technology Management
Blue light from screens suppresses melatonin production. Stop using phones, tablets, and computers one hour before bed.
Enable night mode on devices if evening use is necessary. Position screens at least arm’s length away. Lower brightness settings substantially.
Substance Awareness
Alcohol disrupts sleep architecture despite initial sedation. Limit consumption and avoid drinking within three hours of bedtime.
Nicotine acts as a stimulant. Smokers should avoid cigarettes in the evening hours. Quitting smoking improves sleep quality significantly.
Daytime Light Exposure
Get bright light exposure early in the day. This strengthens circadian rhythm and promotes better nighttime sleep.
Spend at least 30 minutes outside during morning hours. Natural sunlight provides the strongest circadian rhythm cues.
Medical Prevention Strategies
Regular health monitoring helps identify sleep disorder risk factors early. Address underlying conditions before they affect sleep.
Maintain healthy weight through balanced diet and regular exercise. Excess weight significantly increases sleep apnea risk. Even moderate weight loss improves symptoms.
Monitor blood pressure and manage cardiovascular health. Heart conditions and sleep disorders often coexist. Treating one improves the other.
Discuss sleep concerns with your primary care physician during routine visits. Early identification of problems enables faster intervention.
Is Treatment Really Helpful? What Doctors Are Saying
Treatment effectiveness for sleep disorders has improved dramatically in recent decades. Modern sleep medicine offers multiple evidence-based interventions that produce significant results.

Medical Professional Perspectives
Sleep medicine specialists report high success rates across most sleep disorder categories. The American Academy Sleep Medicine emphasizes that proper diagnosis and individualized treatment plans achieve excellent outcomes.
“The vast majority of sleep disorders are highly treatable. We see patients transform their lives once they receive appropriate care. The challenge is getting people to recognize they need help and seek treatment.”
Primary care physicians increasingly recognize sleep disorders as critical health concerns. Many now routinely screen patients for common conditions like insomnia and sleep apnea during annual exams.
Treatment Approaches That Work
Cognitive Behavioral Therapy for Insomnia
Therapy represents the gold standard treatment for chronic insomnia. This structured program addresses thoughts and behaviors that prevent good sleep.
Research shows that 70-80% of patients experience significant improvement. Benefits persist long-term without continued treatment. Many patients reduce or eliminate sleep medications after completing therapy.
The therapy typically involves six to eight sessions with a trained sleep specialist. Components include sleep restriction, stimulus control, and cognitive restructuring.
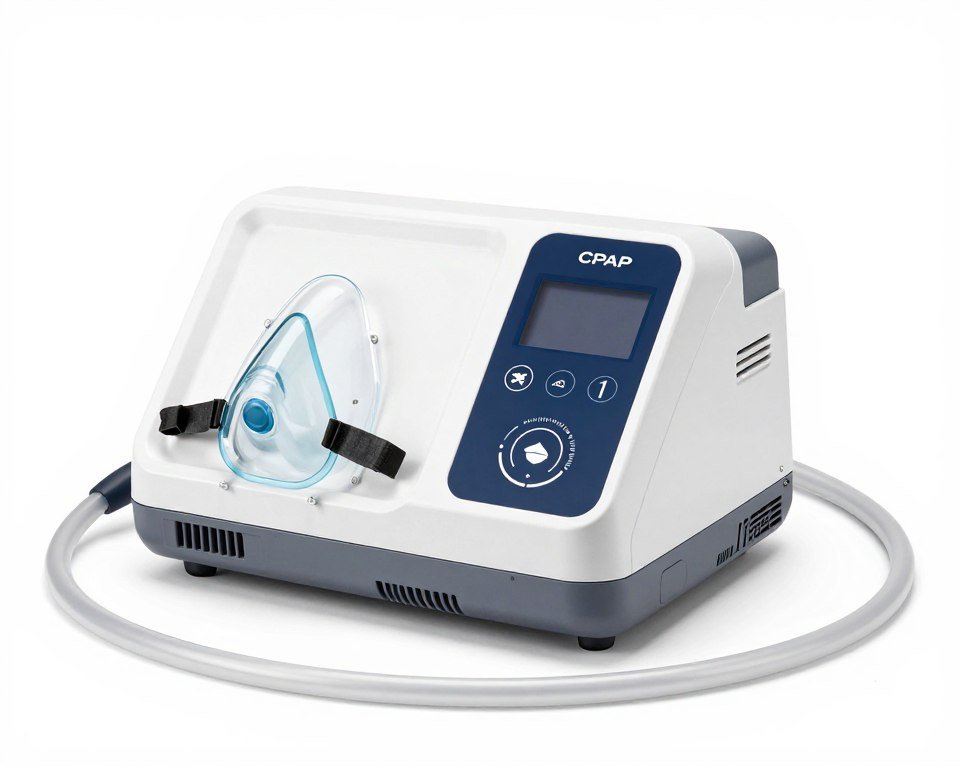
Continuous Positive Airway Pressure for Sleep Apnea
Continuous positive airway pressure therapy effectively treats obstructive sleep apnea. This device delivers steady air pressure through a mask, keeping airways open during sleep.
Studies demonstrate that consistent airway pressure use reduces apnea events by 90% or more. Patients report dramatic improvements in energy, mood, and quality of life.
The American Academy Sleep Medicine recommends continuous positive airway pressure as first-line therapy for moderate to severe sleep apnea. Success requires proper mask fitting and adjustment period.
Medications When Appropriate
Medications play important roles in sleep disorder treatment. Doctors prescribe medications strategically for specific conditions and situations.
Short-term medication use can break insomnia cycles. Newer medications work with natural sleep processes rather than simply sedating patients. Many have minimal side effects when used correctly.
Restless legs syndrome responds well to specific medications that increase dopamine activity. Patients often experience complete symptom relief with proper dosing.
Combination Approaches Maximize Results
Most effective treatment plans combine multiple interventions. Addressing sleep disorders from several angles produces better outcomes than single-approach therapy.
A typical comprehensive plan might include behavioral changes, therapy, medical devices, and when needed, medications. Treatment adjusts based on patient response and changing needs.
Barriers to Treatment Success
Treatment works when patients commit to the process. However, several obstacles prevent people from achieving optimal results.
Non-adherence represents the biggest challenge. Many patients stop using continuous positive airway pressure devices or abandon therapy programs prematurely. Education about long-term benefits improves compliance.
Some patients have unrealistic expectations about treatment timelines. Behavioral interventions require time to produce results. Improvements typically emerge gradually over weeks or months.
Cost concerns prevent some people from pursuing or continuing treatment. Working with insurance providers and exploring payment options can address these barriers.
Sleep Disorders Statistics: 100 Years of Data
Historical trends reveal increasing sleep disorder prevalence throughout the past century. Medical understanding and diagnostic capabilities have evolved dramatically during this period.
Early decades saw limited recognition of sleep disorders as medical conditions. Most people attributed sleep problems to personal weakness or moral failing. Scientific sleep medicine emerged slowly beginning in the 1950s.
The discovery of REM sleep in 1953 revolutionized understanding of sleep processes. This breakthrough enabled researchers to study sleep disorders systematically.
| Decade | Estimated Prevalence | Recognition Level | Key Developments | Primary Diagnosed Conditions |
| 1920s | 5-8% | Very Low | Sleep viewed as passive state | Narcolepsy cases documented |
| 1930s | 8-10% | Very Low | First EEG recordings of sleep | Sleep walking, night terrors |
| 1940s | 10-12% | Low | Barbiturates used for insomnia | War-related sleep disturbances |
| 1950s | 12-15% | Emerging | REM sleep discovered (1953) | Narcolepsy, basic insomnia |
| 1960s | 15-18% | Growing | First sleep disorder clinics open | Insomnia, narcolepsy |
| 1970s | 18-22% | Moderate | Sleep apnea identified, CPAP invented | Sleep apnea, insomnia |
| 1980s | 22-26% | Increasing | AASM founded, sleep medicine specialty | Multiple disorder types recognized |
| 1990s | 26-30% | High | Board certification in sleep medicine | Full range of sleep disorders |
| 2000s | 30-35% | Widespread | Home sleep testing available | Comprehensive diagnosis protocols |
| 2010s | 35-40% | Very High | Digital health tracking widespread | All categories widely diagnosed |
| 2020s | 40-45% | Critical Health Priority | Telemedicine, AI diagnostics, pandemic impact | Record high diagnosis rates |
Factors Driving Increased Prevalence
Multiple factors explain rising sleep disorder rates over the past century. Some increases reflect better recognition and diagnosis rather than new cases.
Modern lifestyle changes contribute significantly. Artificial lighting disrupts natural circadian rhythm cues. The 24/7 economy creates irregular work schedules. Technology use before bed interferes with sleep onset.
Rising obesity rates particularly impact sleep apnea prevalence. Excess weight around the neck constricts airways during sleep. The obesity epidemic and sleep apnea epidemic mirror each other closely.
Increased stress levels affect sleep quality across the population. Economic pressures, information overload, and social media contribute to anxiety that disrupts rest.
Are Sleep Disorders Temporary or Chronic Conditions?
Sleep disorders exist on a spectrum from brief, self-limiting episodes to chronic, lifelong conditions. Understanding this distinction helps set appropriate expectations for recovery and management.
Acute Sleep Disorders
Acute insomnia affects most people at some point. These brief episodes last days to weeks. Stressful life events typically trigger acute sleep problems.
Common triggers include job changes, relationship problems, moving, illness, or grief. Sleep usually normalizes once the stressor resolves or the person adapts.
Acute conditions become concerning when they persist beyond three months. At this point, sleep problems may transition to chronic disorders requiring professional intervention.
Chronic Sleep Disorders
Chronic conditions persist for three months or longer. These disorders require ongoing management rather than quick fixes. Many people live with chronic sleep disorders for years or decades.
Sleep apnea represents a primarily chronic condition. Structural or physiological factors cause this disorder. Without treatment, sleep apnea persists indefinitely.
Chronic insomnia develops when acute sleep problems become entrenched. Negative thought patterns and maladaptive behaviors perpetuate sleep difficulties. These patterns resist change without structured intervention.
Temporary Disorder Characteristics
- Duration less than three months
- Clear triggering event
- Resolves without treatment
- No structural causes
- Normal sleep returns spontaneously
Chronic Disorder Characteristics
- Persists beyond three months
- May lack clear trigger
- Requires active treatment
- Often has underlying causes
- Needs ongoing management
- Risk of relapse exists
- Impacts multiple life areas
- May involve multiple conditions
Factors Determining Chronicity
Several factors influence whether sleep disorders become chronic. Genetics play roles in some conditions. Family history of insomnia or sleep apnea increases individual risk.
Early intervention prevents many acute problems from becoming chronic. Addressing sleep difficulties promptly stops negative patterns from forming.
Underlying health conditions often perpetuate sleep disorders. Chronic pain, respiratory disease, and mental health disorders can maintain sleep problems indefinitely.
Management Versus Cure
Some chronic sleep disorders require lifelong management rather than cure. Sleep apnea patients may need continuous positive airway pressure therapy indefinitely. Discontinuing treatment typically causes symptoms to return.
Other conditions can achieve lasting resolution with proper treatment. Many people with chronic insomnia recover completely after therapy. They maintain normal sleep without ongoing treatment.
Circadian rhythm disorders sometimes improve with life phase changes. Delayed sleep phase disorder common in adolescence often resolves in adulthood as schedules stabilize.
Important distinction: “Chronic” means long-lasting, not untreatable. Many chronic sleep disorders respond excellently to treatment. Patients can achieve normal sleep and quality of life with proper care, even when ongoing management remains necessary.
What Lifestyle Habits Lead to Sleep Disorders?
Daily habits profoundly influence sleep quality. Many sleep disorders develop gradually through accumulated lifestyle factors rather than sudden onset.

Irregular Sleep Schedules
Inconsistent sleep and wake times disrupt circadian rhythm. Weekend schedule changes of more than two hours confuse the body’s internal clock.
Shift work particularly damages sleep health. Rotating shifts prevent adaptation to any consistent schedule. Night shift workers face the highest sleep disorder risk.
Social jet lag occurs when work schedules conflict with biological preferences. Late chronotypes forced into early schedules accumulate sleep debt. This mismatch increases disorder risk substantially.
Poor Bedroom Environment
Environmental factors either support or sabotage sleep. Many Americans sleep in conditions incompatible with quality rest.
Excessive bedroom temperature prevents deep sleep. Most people keep rooms too warm. The body needs to cool slightly to initiate sleep. Temperatures above 70°F interfere with this process.
Light pollution disrupts melatonin production. Street lights, electronics, and device screens signal the brain to stay alert. Even small amounts of light can fragment sleep.
Noise interrupts sleep cycles throughout the night. Traffic, neighbors, pets, and household sounds cause brief arousals. People often don’t remember these awakenings but experience reduced sleep quality.
Substance Use Patterns
Caffeine consumption affects sleep more than most people realize. This stimulant has a half-life of six hours. Afternoon coffee still impacts sleep at bedtime.
Many Americans consume excessive caffeine daily. Energy drinks, coffee, tea, and soft drinks accumulate throughout the day. Total intake often exceeds 400mg, well above recommended limits for good sleep.
Alcohol use for sleep inducement backfires consistently. While alcohol initially causes sedation, it prevents deep restorative sleep. The body metabolizes alcohol during the night, causing middle-of-night awakenings.
Nicotine acts as a stimulant despite some relaxing effects. Smokers experience more fragmented sleep and lighter sleep stages. Withdrawal symptoms can cause early morning awakening.
Diet Timing Issues
Large meals close to bedtime force the body to focus on digestion rather than sleep preparation. Heavy, spicy, or fatty foods cause particular problems.
Eating too little can also disrupt sleep. Going to bed hungry triggers stress hormones that prevent deep sleep.
Exercise Timing
Vigorous exercise within four hours of bed raises body temperature and alertness. This timing conflicts with natural evening wind-down processes.
Sedentary lifestyles also harm sleep quality. Complete lack of physical activity reduces sleep drive and prevents fatigue.
Screen Time Habits
Blue light from devices suppresses melatonin production for hours. Most people use screens right until bedtime or even in bed.
Engaging content keeps the mind active. Social media, news, and entertainment stimulate rather than relax the brain.
Stress and Mental Load
Chronic stress represents one of the most significant lifestyle factors contributing to sleep disorders. Work pressures, financial worries, and relationship problems activate stress response systems incompatible with sleep.
Rumination at bedtime prevents sleep onset. Racing thoughts about past events or future concerns keep the mind engaged. This mental activity signals the body to remain alert.
Lack of relaxation practices means stress accumulates throughout the day. Without deliberate wind-down periods, people carry tension into bed. The body remains in high-alert mode incompatible with rest.
Workspace and Lifestyle Boundaries
Working from bed or bedroom blurs environmental boundaries. The brain begins associating the sleep space with work stress and alertness. This conditioning makes it harder to sleep in that environment.
The always-on culture of American work life extends mental engagement into evening hours. Email checking, work calls, and project planning continue right until bedtime.
Lack of true leisure time prevents natural tiredness from developing. When every evening involves productive activities or screen engagement, the body doesn’t experience natural fatigue cycles.
Sleep Habits That Can Change and Improve Sleep Disorders
Specific habit changes produce measurable improvements in sleep quality. These evidence-based practices work for most people when implemented consistently.

The 10-3-2-1-0 Sleep Formula
This practical framework provides clear timing guidelines for sleep-supporting behaviors. Following these rules consistently improves sleep for most people.
- 10 hours before bed: No more caffeine. Stop all coffee, tea, energy drinks, and caffeinated soft drinks.
- 3 hours before bed: No more food or alcohol. Finish dinner and avoid alcoholic beverages.
- 2 hours before bed: No more work. Stop work-related activities and emails.
- 1 hour before bed: No more screens. Turn off phones, tablets, computers, and televisions.
- 0: The number of times you hit snooze. Wake up at your set time without delay.
Create a Powerful Wind-Down Routine
A consistent pre-bed routine signals your body that sleep approaches. This conditioning helps initiate sleep processes naturally.
Start your routine at the same time every night. Consistency trains your body to expect sleep. The routine itself becomes a powerful sleep cue.
Include relaxing activities only. Reading, gentle stretching, meditation, or listening to calm music work well. Avoid anything stimulating or thought-provoking.

Relaxation Practices
Deep breathing exercises calm the nervous system. Try the 4-7-8 technique: breathe in for 4 counts, hold for 7, exhale for 8.
Progressive muscle relaxation systematically releases tension. Tense and release each muscle group from toes to head.

Environment Optimization
Make your bedroom a sleep sanctuary. Remove work materials, exercise equipment, and clutter. Keep only sleep-related items.
Control all light sources. Use blackout curtains, cover LED lights, and keep devices in another room.
Consistency Practices
Maintain identical sleep and wake times seven days per week. This includes weekends and holidays. Consistency strengthens circadian rhythm.
If you can’t sleep within 20 minutes, leave the bedroom. Do a quiet activity until you feel sleepy, then return to bed.
Strategic Light Exposure
Light represents the strongest circadian rhythm regulator. Strategic timing of light exposure optimizes your biological clock.
Get bright light exposure within 30 minutes of waking. Open curtains immediately or spend time outside. Morning light advances your circadian phase and promotes earlier evening sleepiness.
Dim lights progressively throughout the evening. Start reducing artificial light levels two hours before bed. Use lamps instead of overhead lighting.
If evening screen use is unavoidable, enable night mode settings. Reduce brightness to minimum comfortable levels. Maintain maximum distance from screens.
Physical Activity Guidelines
Regular exercise profoundly improves sleep quality. Studies show that 150 minutes of moderate activity per week reduces insomnia symptoms by 65%.
Morning or afternoon exercise works best for most people. Complete vigorous workouts at least four hours before bedtime. Evening exercise can delay sleep onset for some individuals.
Even light activity helps. A 30-minute daily walk improves sleep quality. Consistency matters more than intensity for sleep benefits.
Nutrition for Better Sleep
Certain foods and eating patterns support quality sleep. Strategic nutrition choices complement other sleep hygiene practices.
Foods rich in tryptophan, magnesium, and melatonin may improve sleep. Turkey, nuts, seeds, cherries, and bananas contain sleep-supporting compounds.
Avoid heavy, spicy, or fatty meals within three hours of bedtime. These foods require extensive digestion that interferes with sleep onset.
Small carbohydrate-based snacks can help some people sleep. A piece of toast or small bowl of cereal may prevent hunger-related awakenings.
Sleep hygiene success tip: Implement one or two changes at a time. Trying to overhaul all habits simultaneously often leads to failure. Build sustainable habits gradually over weeks and months.
Moving Forward with Sleep Disorder Management
Sleep disorders USA represent a significant but manageable health challenge. Understanding these conditions empowers people to seek appropriate help and implement effective strategies.
The past century has brought remarkable advances in sleep medicine. Continuous positive airway pressure therapy, cognitive behavioral therapy for insomnia, and other treatments offer real solutions. Success rates continue improving as research expands knowledge.
Prevention remains the most effective approach. Strong sleep hygiene practices protect against disorder development. Even small habit changes produce measurable benefits over time.
Professional treatment works when prevention isn’t enough. Sleep medicine specialists provide comprehensive care tailored to individual needs. Most people experience significant improvement with proper diagnosis and treatment.
Taking the first step matters most. Whether that means implementing better sleep habits, tracking sleep patterns, or consulting a specialist, action creates change. Quality sleep isn’t a luxury but a fundamental health requirement.
The American Academy Sleep Medicine and other professional organizations continue advancing the field. New treatments emerge regularly. Understanding and resources for sleep disorders have never been more accessible.
Your sleep health deserves priority. The consequences of untreated sleep disorders extend far beyond tiredness. Addressing these conditions improves physical health, mental well-being, relationships, and overall quality of life.







