Liver Disease: The Silent Epidemic Threatening American Health
Liver disease has emerged as one of America’s most pressing health crises. This silent threat affects millions of Americans each year. The liver performs over 500 vital functions in your body. When it fails, the consequences can be devastating.
Many people don’t realize they have liver disease until serious damage occurs. The disease progresses quietly for years. By the time symptoms appear, significant harm may already exist. Understanding this threat is your first step toward protection.
This comprehensive guide explores why liver disease has become a major health emergency in the United States. You’ll discover which age groups face the highest risk. We’ll examine prevention strategies that work. Most importantly, you’ll learn the lifestyle changes that can save your liver.
What Is Liver Disease? Understanding the Basics
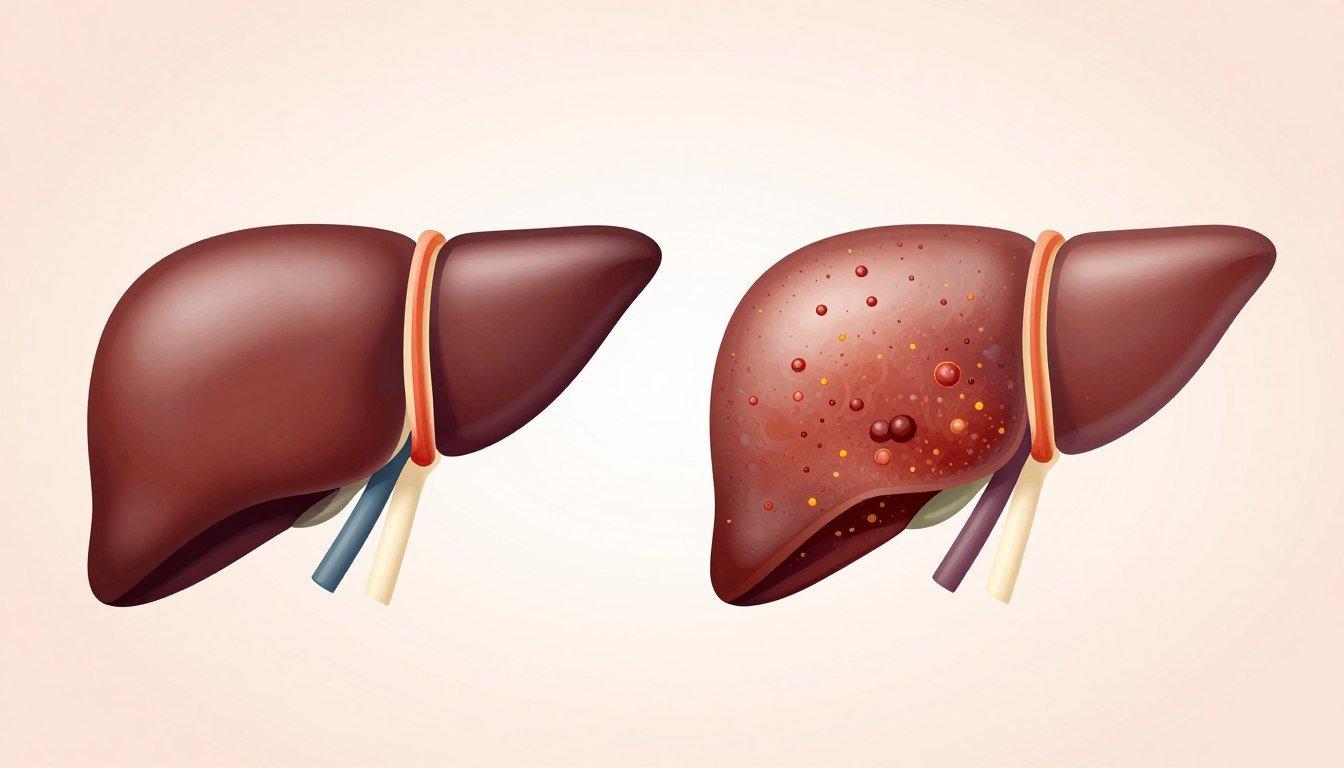
Liver disease encompasses any condition that damages your liver and prevents it from functioning properly. The liver is your body’s largest internal organ. It sits in the upper right side of your abdomen. This powerhouse organ filters toxins from blood. It produces bile for digestion. It stores energy and creates essential proteins.
When disease strikes the liver, these critical functions deteriorate. Liver disease progresses through several stages. Early stages involve inflammation and fatty liver disease. Without intervention, the condition advances to fibrosis. Scar tissue begins replacing healthy liver tissue.
Types of Liver Disease
- Fatty liver disease – excess fat accumulation in liver cells
- Viral hepatitis – infection from hepatitis viruses A, B, or C
- Cirrhosis – advanced scarring and liver damage
- Liver cancer – malignant tumor growth in liver tissue
- Wilson disease – copper buildup causing liver damage
- Autoimmune hepatitis – immune system attacks liver cells
How Liver Disease Develops
The disease progression follows a predictable pattern. First, inflammation damages liver cells. The body responds by creating scar tissue. This fibrosis gradually replaces healthy tissue. Eventually, cirrhosis develops when scarring becomes extensive.
Blood vessels and bile ducts become compromised. The portal vein that carries blood to the liver faces increased pressure. This portal hypertension creates dangerous complications. Blood flow problems lead to bleeding risks.
Chronic liver disease develops over many years. Some types of liver damage prove reversible with early intervention. Advanced disease often becomes permanent. This makes early detection absolutely critical for successful treatment.
Which Age Groups Face the Highest Risk?

Liver disease doesn’t discriminate by age, but certain groups face elevated risks. The disease affects Americans across the entire age spectrum. However, specific age-related patterns have emerged over recent decades.
Middle-Aged Adults (35-54 Years)
This age group experiences the fastest-growing rates of chronic liver disease. Fatty liver disease affects nearly 40% of Americans in this range. Years of dietary habits catch up during these decades. Alcohol use accumulates its damage. Metabolic syndrome becomes prevalent.
Many in this group have undiagnosed hepatitis infections. They contracted these viral infections in their youth. The viruses silently damaged their liver for decades. Symptoms often don’t appear until liver function significantly declines.
Older Adults (55-75 Years)
Older Americans face the highest rates of liver cancer and liver failure. Their livers have endured decades of exposure to risk factors. Cirrhosis reaches its most severe stages in this population. The complications of chronic liver disease manifest most dramatically.
This group also faces challenges from medication interactions. Multiple prescriptions stress already compromised liver function. The body’s ability to regenerate liver tissue decreases with age. Treatment becomes more complex and outcomes less predictable.
Emerging Concern: Young adults aged 25-34 now show alarming increases in fatty liver disease. Obesity rates among younger Americans drive this trend. Early-onset type 2 diabetes contributes to liver damage. Without lifestyle changes, these individuals face liver failure before age 50.
Children and Adolescents
Pediatric liver disease cases have tripled in the past two decades. Childhood obesity fuels this increase. Fatty liver now affects 10% of American children. Genetic conditions like Wilson disease typically present during adolescence.
Early intervention proves crucial for young patients. Their livers possess remarkable regenerative capacity when damage is caught early. Prevention strategies must start in childhood to avoid adult liver disease.
How Liver Disease Became a Crisis in America
The United States faces an unprecedented liver disease epidemic. Multiple factors converged to create this perfect storm of liver health destruction. The crisis overwhelms healthcare systems across the country.
The Obesity Connection
America’s obesity epidemic directly fuels liver disease rates. Over 70% of American adults are overweight or obese. Excess body fat doesn’t just accumulate under the skin. It infiltrates the liver, creating fatty liver disease.
This fatty infiltration triggers inflammation. The inflammatory process damages liver cells. Without intervention, inflammation progresses to fibrosis and cirrhosis. The timeline from fatty liver to cirrhosis now averages just 10-15 years.
Alcohol Consumption Patterns
Alcohol-related liver disease has surged dramatically. Binge drinking among Americans increased by 25% in the past decade. Heavy alcohol use causes direct liver damage. The liver metabolizes alcohol into toxic compounds.
These toxins destroy liver cells and trigger scar tissue formation. Chronic alcohol exposure prevents liver regeneration. The combination of obesity and alcohol use accelerates disease progression. Many patients develop cirrhosis before age 40.
Contributing Lifestyle Factors
- Sedentary behavior and lack of exercise
- High-sugar and processed food consumption
- Chronic stress affecting metabolic health
- Poor sleep patterns disrupting liver function
- Environmental toxin exposure
Healthcare System Challenges
- Late-stage diagnosis when symptoms appear
- Limited access to preventive screening
- Insurance coverage gaps for treatment
- Shortage of liver transplant organs
- Insufficient public awareness campaigns
The Viral Hepatitis Impact
Hepatitis C virus infected millions of Americans between 1960 and 1990. Many remain undiagnosed today. The virus silently destroys liver tissue for decades. Baby boomers carry the highest infection rates.
While treatments now cure hepatitis C, many infected individuals don’t know their status. Untreated viral hepatitis leads to cirrhosis and liver cancer. The opioid epidemic introduced new hepatitis infection routes. Needle sharing spreads the virus among younger populations.
Stress and Mental Health
Chronic stress affects liver health in multiple ways. Stress hormones alter metabolism and promote fat storage in the liver. Americans report record-high stress levels. The pandemic intensified mental health challenges and unhealthy coping mechanisms.
Stress-related alcohol use and emotional eating damage liver tissue. Depression and anxiety reduce motivation for healthy lifestyle choices. The mind-body connection plays a crucial role in liver disease development.
Medical professionals report feeling overwhelmed: Hospital liver disease units operate at 110% capacity nationwide. Transplant waiting lists have doubled in five years. Emergency departments see acute liver failure cases weekly instead of monthly.
How to Prevent Liver Disease: Proven Strategies
Prevention remains your most powerful weapon against liver disease. You possess more control over your liver health than you might realize. Simple daily choices compound into significant long-term protection.
Maintain a Healthy Weight
Achieving and maintaining a healthy body weight protects your liver from fatty infiltration. Even modest weight loss delivers substantial benefits. Losing just 7-10% of body weight can reverse fatty liver disease completely.
Weight loss reduces inflammation in liver tissue. Scar tissue formation slows or stops. The liver regains its ability to perform essential functions. Sustainable weight management prevents disease recurrence.
Limit Alcohol Consumption
Alcohol abstinence or strict moderation prevents alcohol-related liver damage. Men should limit intake to two drinks daily maximum. Women should consume no more than one drink per day. These limits allow the liver time to process alcohol safely.
Complete abstinence provides optimal liver protection. If you drink, avoid binge drinking episodes. Give your liver alcohol-free days each week. Early alcohol cessation allows damaged liver tissue to regenerate.
Dietary Prevention
- Eat plenty of fruits and vegetables
- Choose whole grains over refined carbohydrates
- Select lean protein sources
- Limit saturated and trans fats
- Reduce sugar consumption
- Stay hydrated with water
Exercise Guidelines
- Aim for 150 minutes weekly moderate activity
- Include both cardio and strength training
- Start slowly and build gradually
- Find activities you enjoy
- Make movement part of daily routine
- Consider walking as accessible exercise
Medical Prevention
- Get vaccinated against hepatitis A and B
- Regular screening if at risk
- Practice safe sex to prevent infections
- Avoid sharing needles or personal items
- Discuss medications with your doctor
- Monitor over-the-counter drug use
Avoid Toxin Exposure
Your liver filters countless substances daily. Minimizing toxin exposure reduces this burden. Be cautious with cleaning chemicals and pesticides. Use proper ventilation when handling toxic substances.
Many medications stress the liver. Acetaminophen overdose causes acute liver failure. Follow dosing instructions carefully. Never combine acetaminophen with alcohol. Discuss all medications and supplements with healthcare providers.
Regular Health Screenings
Early detection catches liver disease before irreversible damage occurs. Ask your doctor about liver function tests. These blood tests measure liver enzyme levels. Elevated enzymes signal liver inflammation or damage.
People at high risk need annual screening. Risk factors include obesity, diabetes, family history, and past alcohol abuse. Hepatitis screening identifies viral infections early. Modern treatments cure hepatitis C before cirrhosis develops.
100 Years of Liver Disease in America: The Numbers
The history of liver disease in America reveals dramatic changes over the past century. Medical advances improved some outcomes. Lifestyle changes worsened others. These statistics tell a compelling story of progress and setbacks.
| Decade | Cases per 100,000 | Mortality Rate | Primary Cause | Major Development |
| 1920-1930 | 45 | 12.3 | Infections | Limited treatment options |
| 1930-1940 | 52 | 14.1 | Alcohol abuse | Prohibition repeal impacts |
| 1940-1950 | 48 | 13.5 | Viral hepatitis | War-related blood transfusions |
| 1950-1960 | 55 | 15.8 | Hepatitis B | First liver function tests |
| 1960-1970 | 62 | 17.2 | Hepatitis spread | Hepatitis B virus identified |
| 1970-1980 | 71 | 18.9 | Drug use hepatitis | First liver transplant success |
| 1980-1990 | 85 | 21.4 | Hepatitis C epidemic | Hepatitis C discovered |
| 1990-2000 | 98 | 24.6 | Hepatitis C, alcohol | Improved transplant outcomes |
| 2000-2010 | 124 | 28.3 | Fatty liver disease | Obesity epidemic begins |
| 2010-2020 | 156 | 32.7 | Non-alcoholic fatty liver | Hepatitis C cure developed |
| 2020-Present | 187 | 36.2 | Metabolic disease | COVID-19 impacts liver health |
These statistics reveal troubling trends. Liver disease cases increased by over 300% in the past century. Mortality rates tripled despite medical advances. The shift from infectious causes to metabolic disease reflects changing American lifestyles.
The steepest increases occurred after 2000. This timeline matches the obesity epidemic’s acceleration. Fatty liver disease replaced viral hepatitis as the leading cause. The trend shows no signs of slowing without major intervention.
Critical Projection: Current trends suggest liver disease cases could reach 250 per 100,000 by 2030. Mortality rates may exceed 45 per 100,000. These numbers represent a genuine public health emergency requiring immediate action.
Is Treatment Really Helpful? What Works for Liver Disease

Treatment effectiveness depends heavily on disease stage and type. Early intervention produces remarkable results. Advanced disease requires more aggressive approaches. The good news: modern medicine offers more options than ever before.
Early-Stage Treatment Success
Fatty liver disease responds exceptionally well to lifestyle intervention. Studies show 70-90% of patients reverse fatty liver through weight loss and diet changes. The liver possesses remarkable regenerative capacity when damage is caught early.
Viral hepatitis treatment has revolutionized outcomes. New antiviral medications cure hepatitis C in over 95% of cases. These treatments take just 8-12 weeks. They prevent progression to cirrhosis and liver cancer. Early treatment saves lives and restores liver function.
Managing Chronic Liver Disease
Chronic liver conditions require ongoing management. Medications control inflammation and slow disease progression. Regular monitoring catches complications early. Dietary modifications reduce strain on compromised liver function.
Treatment plans must address underlying causes. Alcohol cessation stops alcohol-related damage. Diabetes control prevents further fatty liver progression. Managing risk factors prevents additional liver injury.
Advanced Disease Treatment
Cirrhosis requires comprehensive medical management. Doctors monitor for complications like portal hypertension and bleeding. Medications reduce fluid buildup and infection risk. Treatment focuses on maintaining remaining liver function.
Liver cancer treatment depends on tumor size and liver function. Early-stage tumors may be removed surgically. Ablation therapy destroys small tumors. Advanced cases may require liver transplant. Five-year survival rates have improved dramatically with modern treatment protocols.
Liver Transplant Outcomes
Liver transplant offers hope for end-stage liver failure patients. Transplant technology and techniques have advanced significantly. One-year survival rates now exceed 90%. Five-year survival reaches 75-80%.
The major challenge remains organ shortage. Over 17,000 Americans await liver transplant. Only 8,000 transplants occur annually. Living donor transplants provide alternatives. A healthy person can donate part of their liver safely.
Emerging Therapies
Research continues advancing liver disease treatment. New medications target liver fibrosis directly. These drugs may reverse scar tissue formation. Clinical trials show promising results for fatty liver disease treatments.
Regenerative medicine explores growing liver tissue in laboratories. Stem cell therapies may repair damaged liver cells. Gene therapy shows potential for genetic liver conditions. These innovations offer hope for currently untreatable conditions.
What Doctors Are Saying About the Liver Disease Crisis

Medical professionals on the front lines express deep concern about liver disease trends. Their insights reveal the crisis magnitude and treatment challenges. These expert perspectives shape public health strategies.
“We’re seeing patients in their thirties with cirrhosis that we used to only see in sixty-year-olds. The combination of obesity and alcohol use is devastating. Many don’t realize they have liver disease until it’s too late for reversal.”
Prevention as Primary Strategy
Doctors emphasize prevention over treatment. Liver specialists stress that preventing disease proves far easier than reversing damage. They advocate for aggressive public health campaigns. Early screening programs could identify at-risk individuals before symptoms develop.
Healthcare providers express frustration over late-stage diagnoses. Most patients seek care only after experiencing symptoms. By then, liver damage is often irreversible. Doctors call for routine liver function screening in annual checkups.
“The liver disease epidemic mirrors the obesity crisis. We can’t treat our way out of this problem. We need societal changes promoting healthy eating and active lifestyles. Prevention must become our priority.”
Treatment Access Challenges
Medical professionals highlight treatment access barriers. Hepatitis C medications cost thousands of dollars. Insurance coverage varies significantly. Many patients can’t afford life-saving treatments. This disparity creates preventable deaths.
Rural Americans face particular challenges accessing liver specialists. Transplant centers concentrate in major cities. Travel requirements burden patients already weakened by disease. Telemedicine expands access but can’t replace hands-on care.
Lifestyle Medicine Integration
Progressive doctors integrate lifestyle medicine into treatment plans. They prescribe specific diets and exercise programs. Behavioral health support addresses underlying issues. This comprehensive approach improves outcomes significantly.
Some clinics offer intensive lifestyle intervention programs. Patients receive nutrition counseling, fitness coaching, and psychological support. Results show dramatic improvements in liver function. Many patients avoid medication or transplant through intensive lifestyle changes.
Key Medical Recommendations
- Annual liver function screening for at-risk populations
- Immediate lifestyle intervention at first signs of fatty liver
- Aggressive hepatitis screening and treatment
- Multidisciplinary care teams for chronic liver patients
- Mental health support as standard care component
- Patient education emphasizing prevention and early intervention
“Every day of delay in treating liver disease matters. The liver can regenerate remarkably well if we catch problems early. Patient education and regular screening would prevent most cases of advanced liver disease we see.”
Reversible or Chronic? Understanding Your Liver’s Healing Potential
The question of reversibility depends entirely on disease stage and type. The liver possesses unique regenerative abilities. This organ can regrow to full size from just 25% of original tissue. However, this remarkable capacity has limits.
Reversible Liver Conditions
Fatty liver disease in its early stages proves completely reversible. When you eliminate the cause, the liver clears accumulated fat. Normal liver function returns within months. Studies confirm that weight loss and lifestyle changes restore liver health entirely.
Mild to moderate fibrosis can reverse with proper treatment. Stopping alcohol consumption allows scar tissue to resolve gradually. Treating viral hepatitis prevents further scarring. The liver slowly replaces scar tissue with healthy cells.
Conditions That Can Reverse
- Simple fatty liver (steatosis)
- Mild liver inflammation (hepatitis)
- Early-stage fibrosis
- Drug-induced liver injury (when stopped)
- Alcohol-related damage (with abstinence)
- Viral hepatitis (with treatment)
Typically Irreversible Conditions
- Advanced cirrhosis
- End-stage liver failure
- Severe scar tissue formation
- Liver cancer (advanced stages)
- Chronic autoimmune hepatitis damage
- Genetic liver diseases (require management)
The Cirrhosis Turning Point
Cirrhosis represents the point of no return for liver disease. Once extensive scarring develops, reversal becomes impossible. The scar tissue permanently replaces functional liver cells. Blood vessels and bile ducts suffer permanent damage.
However, even cirrhosis progression can be halted. Stopping the damaging process prevents further deterioration. Remaining liver function can be preserved. Many cirrhosis patients live years with proper management.
Compensated cirrhosis means the liver still functions adequately despite scarring. Decompensated cirrhosis indicates liver failure. The body can no longer maintain essential functions. This stage requires transplant evaluation.
Factors Affecting Reversibility
Several factors determine whether liver damage can reverse. Age plays a significant role. Younger livers regenerate more efficiently. The extent of existing damage matters greatly. Early intervention produces better outcomes.
Continued exposure to damaging factors prevents healing. Ongoing alcohol use blocks regeneration. Persistent obesity maintains fatty infiltration. Eliminating harmful factors gives your liver the best chance to heal.
Genetic factors influence regenerative capacity. Some people heal faster than others. Nutritional status affects healing speed. Adequate protein and vitamins support liver regeneration. Underlying health conditions can slow recovery.
Chronic Management Strategies
When reversal isn’t possible, chronic disease management becomes essential. Regular monitoring catches complications early. Medication prevents disease progression. Lifestyle modifications improve quality of life.
Chronic liver disease patients need comprehensive care teams. Hepatologists manage medical treatment. Nutritionists optimize diet for liver function. Mental health professionals address depression and anxiety. Social workers connect patients with resources.
Many chronic liver disease patients maintain good quality of life for years. The key lies in consistent medical care and lifestyle adherence. Regular follow-up appointments ensure problems are caught early. Medication compliance prevents complications.
Food and Alcohol Habits That Destroy Your Liver

Your daily food and drink choices directly impact liver health. Some habits inflict serious damage over time. Understanding these risks empowers you to make protective choices. Small changes compound into significant liver protection.
Alcohol’s Direct Liver Damage
Alcohol metabolism creates toxic compounds that directly damage liver cells. The liver prioritizes processing alcohol over other functions. This metabolic burden stresses liver tissue. Chronic alcohol exposure overwhelms the liver’s repair mechanisms.
Heavy drinking causes fatty liver within weeks. Continued use progresses to alcoholic hepatitis. Inflammation damages liver structure. Without cessation, cirrhosis develops. The timeline accelerates with binge drinking patterns.
- Daily consumption exceeding recommended limits
- Binge drinking episodes (5+ drinks in 2 hours)
- Mixing alcohol with medications
- Drinking on empty stomach
- Using alcohol to cope with stress
- Unable to stop after starting
High-Risk Drinking Patterns
- Exceeding 2 drinks daily for men
- Exceeding 1 drink daily for women
- Daily drinking without alcohol-free days
- Consuming alcohol with fatty meals
- Drinking during medication use
- Social drinking several times weekly
Moderate-Risk Behaviors
- Staying within recommended limits
- Including multiple alcohol-free days
- Drinking with food
- Staying hydrated with water
- Avoiding binge drinking
- Choosing lower alcohol content options
Liver-Safe Practices
Sugar and Processed Carbohydrates
Excessive sugar consumption drives fatty liver disease development. The liver converts excess sugar into fat. This fat accumulates within liver cells. High fructose corn syrup proves particularly damaging.
Processed carbohydrates spike blood sugar rapidly. Insulin levels surge in response. High insulin promotes fat storage in the liver. This metabolic dysfunction creates and worsens fatty liver disease.
Sugar-sweetened beverages deliver concentrated sugar loads. One soda contains 40+ grams of sugar. Regular consumption dramatically increases liver disease risk. Studies link daily soda intake to doubled fatty liver risk.
Unhealthy Fats and Fried Foods
Trans fats and excessive saturated fats promote liver inflammation. These fats accumulate in liver tissue. They trigger inflammatory responses. Chronic inflammation damages liver cells and accelerates fibrosis.
Fried foods combine multiple risk factors. High fat content, refined carbohydrates, and often excessive sodium stress liver function. Regular fried food consumption correlates strongly with fatty liver disease development.
Foods That Damage Your Liver
- Sugary beverages and sodas
- White bread and refined grains
- Fried foods and fast food
- Processed meats and hot dogs
- Candy and baked goods
- High-sodium processed foods
- Excessive red meat consumption
- Foods with trans fats
Hidden Liver Threats
- Fruit juices (concentrated sugar)
- Flavored yogurts with added sugar
- Granola and “healthy” bars
- Salad dressings with hidden sugars
- Dried fruits (concentrated sugar)
- Specialty coffee drinks
- Condiments high in sugar
- Low-fat products with added sugar
Portion Sizes and Eating Patterns
Overeating burdens liver metabolism regardless of food quality. Large portions spike insulin and promote fat storage. Frequent eating without fasting periods prevents the liver from processing stored fat.
Late-night eating disrupts liver metabolism rhythms. The liver performs repair and detoxification during sleep. Eating close to bedtime interferes with these processes. Studies show late eating increases fatty liver risk.
Nutritional Deficiencies
Poor nutrition compromises liver function in multiple ways. Inadequate protein prevents liver repair. Vitamin deficiencies impair detoxification. Fiber deficiency affects bile production and toxin elimination.
Crash diets and extreme calorie restriction can actually worsen liver health. Rapid weight loss releases stored toxins. The liver becomes overwhelmed processing these substances. Gradual, sustainable weight loss protects liver function.

Lifestyle Changes That Improve Liver Health

Transforming your lifestyle protects and heals your liver. These evidence-based changes deliver measurable improvements. You don’t need perfection. Consistent small steps create lasting results.
Adopt a Liver-Friendly Diet
Mediterranean diet patterns provide optimal liver protection. This eating style emphasizes whole foods, healthy fats, and plant-based meals. Studies show Mediterranean diet followers reduce fatty liver disease risk by 50%.
Focus on nutrient-dense foods that support liver function. Leafy greens contain compounds that aid detoxification. Cruciferous vegetables support liver enzyme production. Berries provide antioxidants that reduce inflammation.
Liver-Supporting Foods
- Leafy greens (spinach, kale)
- Cruciferous vegetables (broccoli, cauliflower)
- Fatty fish (salmon, sardines)
- Nuts and seeds
- Olive oil
- Green tea
- Garlic and onions
- Berries and citrus fruits
Daily Habits for Liver Health
- Drink 8-10 glasses of water
- Eat breakfast within 2 hours of waking
- Include protein at each meal
- Limit eating to 12-hour window
- Choose whole grains over refined
- Prepare meals at home
- Read nutrition labels carefully
- Plan meals in advance
Beneficial Beverages
- Water (primary beverage)
- Green tea (3-4 cups daily)
- Coffee (2-3 cups daily)
- Herbal teas (dandelion, milk thistle)
- Fresh vegetable juices
- Kombucha (in moderation)
- Coconut water
- Lemon water
Exercise for Liver Protection
Regular physical activity directly improves liver health. Exercise reduces liver fat content. It improves insulin sensitivity. Movement helps your body process and eliminate toxins efficiently.
Both aerobic exercise and strength training benefit the liver. Cardio activities burn fat and improve circulation. Resistance training builds muscle that helps regulate blood sugar. Combining both types maximizes liver benefits.
You don’t need intense workouts to see results. Moderate activity provides substantial protection. Walking 30 minutes daily reduces fatty liver disease risk significantly. Consistency matters more than intensity.
Sleep and Stress Management
Quality sleep allows your liver to perform essential repair work. The liver follows circadian rhythms for optimal function. Poor sleep disrupts these patterns. Aim for 7-9 hours nightly for liver health.
Chronic stress damages liver health through multiple mechanisms. Stress hormones promote fat storage in the liver. Stress often leads to unhealthy coping behaviors. Managing stress protects your liver.
Stress Reduction Techniques
- Practice deep breathing exercises daily for 10 minutes
- Try meditation or mindfulness apps
- Engage in regular physical activity you enjoy
- Maintain social connections and support systems
- Limit news and social media exposure
- Pursue hobbies and creative activities
- Consider professional counseling if needed
- Establish boundaries at work and home
Sleep Hygiene Practices
- Maintain consistent sleep and wake times
- Create dark, cool bedroom environment
- Avoid screens 1 hour before bed
- Limit caffeine after 2 PM
- Avoid alcohol close to bedtime
- Don’t eat large meals before sleep
- Exercise earlier in the day
- Use relaxation techniques before bed
Environmental Toxin Reduction
Minimizing toxin exposure reduces your liver’s detoxification burden. Choose natural cleaning products when possible. Improve indoor air quality with plants and ventilation. Filter drinking water to remove contaminants.
Be cautious with personal care products. Many contain chemicals the liver must process. Choose products with minimal ingredients. Avoid unnecessary medications and supplements that stress the liver.
Social Support and Accountability
Lifestyle changes succeed better with support systems. Share your goals with family and friends. Join health-focused groups or classes. Consider working with health coaches or nutritionists.
Track your progress to maintain motivation. Keep food journals or use health apps. Monitor how lifestyle changes affect how you feel. Celebrate small victories along the way.

Taking Action Against America’s Liver Disease Crisis
Liver disease represents one of the most serious health threats facing Americans today. The statistics paint a sobering picture. Cases have more than tripled in the past century. Mortality rates continue climbing despite medical advances.
Yet hope exists within this crisis. The liver possesses remarkable healing capacity when given the chance. Early intervention reverses most damage. Prevention strategies work effectively. Treatment options continue improving.
Your daily choices determine your liver’s fate. The food you eat either protects or damages this vital organ. Your activity level affects liver fat accumulation. Alcohol consumption directly impacts liver tissue. Sleep quality influences liver repair processes.

Small changes compound into significant protection. You don’t need perfection to improve liver health. Walking 30 minutes daily makes a difference. Reducing sugar intake protects your liver. Adding more vegetables supports liver function. These simple steps deliver measurable benefits.
The liver disease crisis demands immediate action at individual and societal levels. Healthcare systems must prioritize prevention and screening. Public health campaigns need to raise awareness. Insurance coverage must improve for life-saving treatments.
As individuals, we control our personal risk factors. Understanding liver disease empowers better choices. Recognizing symptoms enables earlier diagnosis. Committing to lifestyle changes protects this irreplaceable organ.
Don’t wait for symptoms to appear before taking action. Liver disease progresses silently for years. By the time you feel sick, significant damage may already exist. Prevention and early intervention remain your best strategies.
Your liver performs over 500 essential functions every day. It deserves your attention and protection. The choices you make today determine your liver health tomorrow. Take control of your liver health now. Your future self will thank you.